Venous foot ulcers are a growing concern. According to some statistics, the prevalence of venous ulcers in the United States is anywhere between 1 and 22% in individuals aged over 60. [1] Moreover, around 80% of all lower extremity ulcers are due to venous causes. [2] Given the high prevalence of venous ulcers, it is essential for podiatrists and wound care professionals to be aware of effective wound care principles for venous foot ulcers.
What is a Venous Foot Ulcer?
Venous ulcer - historically known as “ venous stasis ulcer” is a chronic, subcutaneous lesion usually present around the medial malleolus (the ‘gaiter area’) in the lower extremities. [3] The presence of venous ulcer is a complication of chronic venous insufficiency and is indicative of severe disease. As venous insufficiency impairs the normal wound healing process, venous foot ulcers are chronic in nature and can be difficult to treat. A multidisciplinary team consisting of wound care specialists, podiatrists, vascular surgeons, and specialist nursing can help provide the necessary effective care to patients with venous ulcers.
Pathophysiology
An understanding of the pathophysiology of venous ulcers can help podiatrists plan effective management for patients with venous foot ulcers. While the exact pathogenesis is not known, venous valve incompetence and “venous hypertension” are said to be the primary cause of venous ulcer development. Factors like immobility, calf muscle pump dysfunction, trauma, and congenital absence of valves can contribute to venous valve incompetence. Subsequently, pooling of venous blood occurs which triggers an inflammatory process ultimately leading to venous ulcer formation.
Clinical Features of Venous Foot Ulcers
It is necessary to distinguish venous ulcers from other ulcer types as the management plan differs according to the etiology. The following characteristic clinical features can help clinicians diagnose venous ulcers:
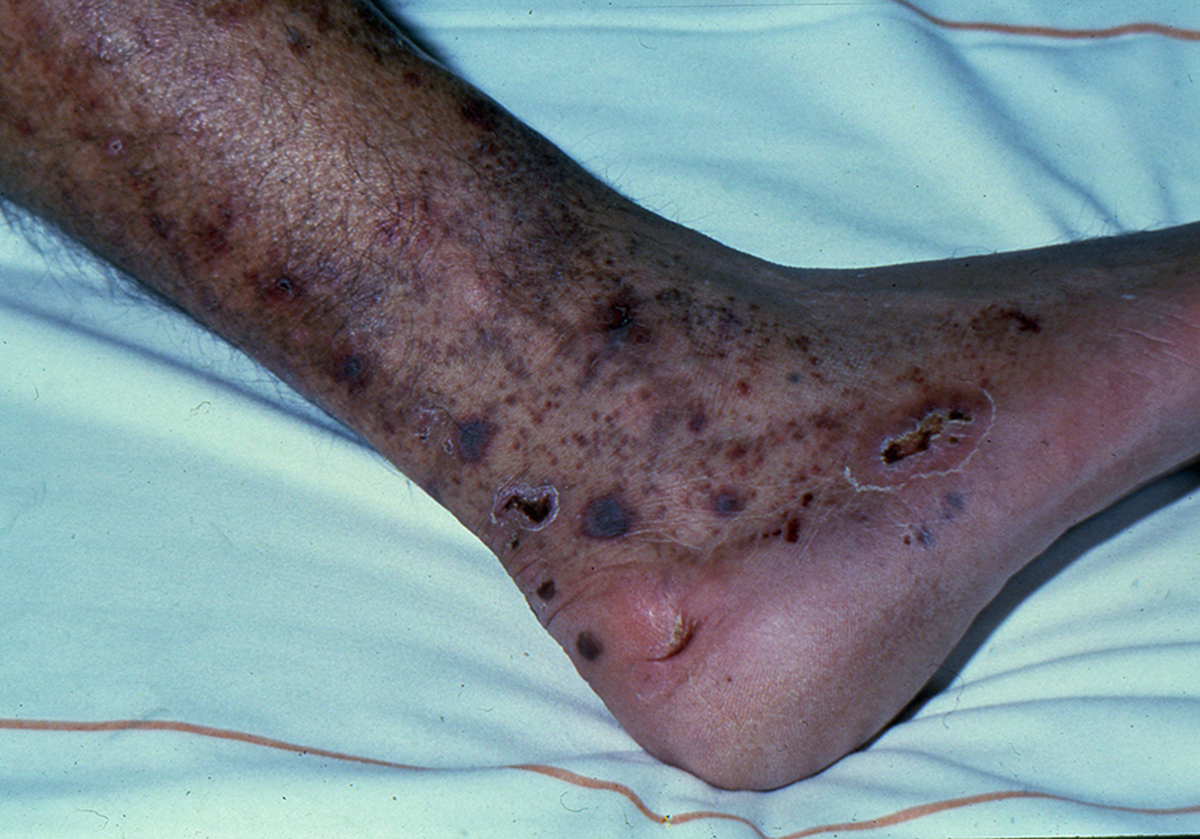
- Shallow ulcers with irregular margins are present in the gaiter region. However, the location can be variable and ulcer might also be present on the lateral malleolus.
- Patients usually have a history of DVT or venous insufficiency.
- Red granulation tissue or exudate is present in the ulcer bed.
- Hemosiderin deposits leading to hyperpigmentation and "lipodermatosclerosis" around the ulcer wound are observed.
- Eczematous changes are seen in the skin near the ulcer edge. [4]
Wound Care Solutions For Venous Ulcers
The principal goal of all wound care solutions is to preserve the tissue from further deterioration. A combination of medical and surgical options are available that can help stimulate the wound healing process.
- Antibiotics: Bacteria in the skin flora can colonize chronic wounds but indiscriminate antibiotic use should be avoided. This is because the use of systemic antibiotics has not been proven to show any reduction in bacterial colonization. [5] The opposite has been observed with the emergence of antibiotic-resistant bacteria. Therefore, antibiotic use should only be reserved for patients exhibiting clinical signs and symptoms of cellulitis or acute wound infection. [6]
- Wound Skin Care: Wounds should be kept clean for optimum healing. In case of dryness, petroleum-based emollients should be used. Normal saline has been found to be the safest for wound irrigation.
- Debridement: The presence of dead, necrotic tissue increases the risk of sepsis and bacterial colonization. Debridement is the removal of nonviable, damaged tissue using surgical, biological, or enzymatic means. This helps stimulate the formation of healthy granulation tissue. While conclusive evidence is still lacking, some studies suggest that serial debridements can improve wound healing time. [7]
- Moist Dressing: Dressings can help provide a moist environment which is considered optimum for wound healing. Exudate, odor, and pain control can also be effectively controlled with an appropriate dressing. An occlusive hydrocolloid dressing is generally used for the management of venous ulcers. Alginate dressings might also have similar efficacy. [8]
- Compression Therapy: Compression therapy might be considered the most important part of venous wound care. Peripheral vascular disease and diabetic neuropathy should be excluded prior to compression therapy. Pressure bandages are applied to the leg with maximal pressure at the gaiter region. As venous foot ulcers co-exist with chronic venous insufficiency, compression therapy helps reverse or minimize the effects of venous insufficiency. Patients who fail to exhibit any improvement with compression therapy should be evaluated for an alternative diagnosis. [9]
- Medical Treatment: Pentoxifylline 400 mg TDS is recommended for the treatment of venous ulcers. [10] Venous stasis dermatitis might also benefit from the local application of steroids. While aspirin has been recommended for the treatment of venous ulcers, sufficient evidence has not yet been discovered. [11]
- Surgery: Surgical options are considered if medical treatments fail to show any improvement. Superficial venous ablation can be effective in managing venous insufficiency. Patients should be referred to vascular specialists for early venous reflux ablation. [12] Reconstructive surgery can also be considered for persistent wounds.
- Other Treatment Options: Intermittent pneumatic compression has been found to reduce the rates of ulcer recurrence in a Cochrane review. [13] Hyperbaric oxygen therapy, on the other hand, has not been proven to improve wound healing [14]
Regular Follow Up and Scope of Telehealth
Patients should be regularly followed up to prevent the recurrence of venous foot ulcers. Unfortunately, the recurrence rate of venous foot ulcers is high. Therefore a regular follow-up with a podiatrist is important. Telehealth consultations can be excellent for providing follow-up care to patients who otherwise might find regular physical appointments tedious. It also allows for a more equitable distribution of health resources and early prevention of ulcer recurrence. [15]
REFERENCES
- Cornwall JV, Doré CJ, Lewis JD. Leg ulcers: epidemiology and aetiology. Br J Surg. 1986;73(9):693–6.
- Collins L, Seraj S. Diagnosis and treatment of venous ulcers. Am Fam Physician. 2010;81(8):989–96.
- Levick JR. Revision of the Starling principle: new views of tissue fluid balance. J Physiol. 2004;557(Pt 3):704.
- Etufugh CN, Phillips TJ. Venous ulcers. Clin Dermatol. 2007;25(1):121–30.
- Alinovi A, Bassissi P, Pini M. Systemic administration of antibiotics in the management of venous ulcers. A randomized clinical trial. J Am Acad Dermatol. 1986;15(2 Pt 1):186–91.
- O’Meara S, Al-Kurdi D, Ologun Y, Ovington LG, Martyn-St James M, Richardson R. Antibiotics and antiseptics for venous leg ulcers. Cochrane Database Syst Rev. 2014;(1):CD003557.
- Cardinal M, Eisenbud DE, Armstrong DG, Zelen C, Driver V, Attinger C, et al. Serial surgical debridement: a retrospective study on clinical outcomes in chronic lower extremity wounds. Wound Repair Regen. 2009;17(3):306–11.
- O’Meara S, Martyn-St James M. Alginate dressings for venous leg ulcers. Cochrane Database Syst Rev. 2013;(4):CD010182.
- O’Meara S, Cullum N, Nelson EA, Dumville JC. Compression for venous leg ulcers. Cochrane Database Syst Rev. 2012;11:CD000265.
- Jull A, Arroll B, Parag V, Waters J. Pentoxifylline for treating venous leg ulcers. Cochrane Database Syst Rev. 2007;(3):CD001733.
- de Oliveira Carvalho PE, Magolbo NG, De Aquino RF, Weller CD. Oral aspirin for treating venous leg ulcers. Cochrane Database Syst Rev. 2016;2:CD009432.
- Gohel MS, Heatley F, Liu X, Bradbury A, Bulbulia R, Cullum N, et al. A randomized trial of early endovenous ablation in venous ulceration. N Engl J Med. 2018;378(22):2105–14.
- Nelson EA, Bell-Syer SEM. Compression for preventing recurrence of venous ulcers. Cochrane Database Syst Rev. 2012;(8):CD002303.
- Kranke P, Bennett MH, Martyn-St James M, Schnabel A, Debus SE, Weibel S. Hyperbaric oxygen therapy for chronic wounds. Cochrane Database Syst Rev. 2015;(6):CD004123.
- Karadag A, Sengul T. Challenges faced by doctors and nurses in wound care management during the COVID-19 pandemic in Turkey and their views on telehealth. J Tissue Viability [Internet]. 2021; Available from: https://linkinghub.elsevier.com/retrieve/pii/S0965-206X(21)00103-0


.webp)

.avif)