Pressure ulcers and injuries are a common occurrence in hospitals. In the U.S., 2.5 million pressure injuries are treated each year which represents a significant burden of disease on the healthcare system. [1]
What Are Pressure Ulcers?
Pressure ulcers - also known as bedsores, pressure injury, or pressure necrosis occur due to localized skin trauma over sites of bony prominence as a result of sustained pressure. These are most commonly seen in chronically-ill, frail individuals who are bed-bound. However, these might also result from the use of ill-fitting casts and other medical equipment. [2] Pressure ulcers are especially common in nursing home residents.
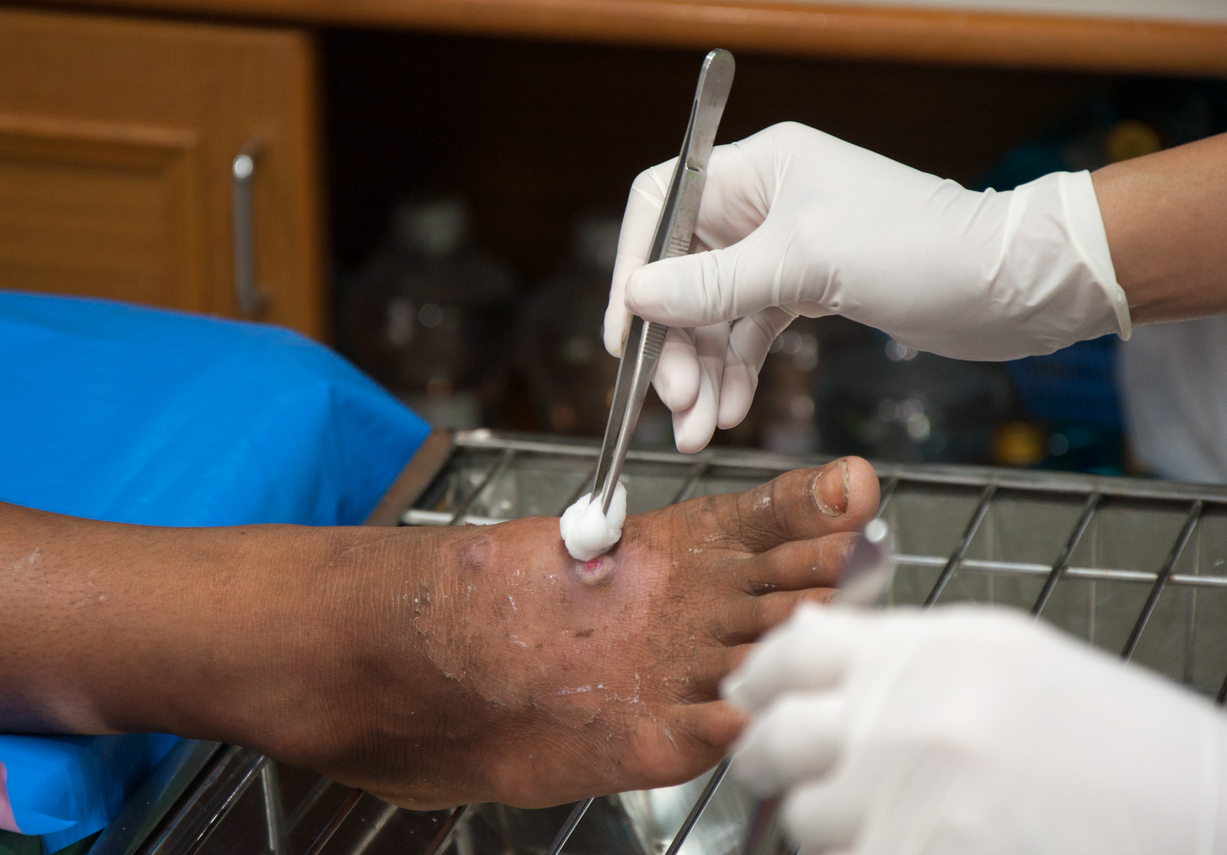
The common sites of pressure ulcers include the hip and sacral region which account for 70% of all pressure ulcers. An additional 15-20% of pressure ulcers occur in the lower extremities. [3] Podiatrists and wound care specialists should therefore regularly assess and examine these regions for the early detection of pressure ulcers.
Why Do Pressure Ulcers Occur?
External sustained pressure can compress the network of capillaries responsible for skin perfusion. The estimated value of this pressure is said to exceed the value of arteriolar pressure (32 mmHg). However, the pressure sufficient to cause ulceration varies amongst individuals. As a result of sustained pressure, tissue hypoxia leads to ischemic changes and necrosis which contribute to skin injury and subsequent ulceration. Poor perfusion impairs the progression of wound healing stages, which leads to the formation of chronic, non-healing ulcers.
Muscles are the most susceptible to pressure-induced injury, followed by the dermis and adipose tissue. Bony prominences are the site of the greatest pressure which explains the distribution of pressure ulcers over these regions. [4]
Risk Factors
Wound care specialists should be aware of the risk factors that can contribute to the development of pressure ulcers. The majority of these risk factors act by impairing the normal wound healing process. With a better knowledge of the risk factors, podiatrists and wound care specialists can provide patients with an individualized preventive treatment plan.
Some of the risk factors associated with pressure ulcers include:
- Immobility: Immobility is the single most likely cause for the development of pressure ulcers. Patients with less spontaneous movements were found to have a higher risk of developing pressure ulcers. [5]
- Malnutrition: Adequate nutrition is essential for wound healing and skin integrity. Malnourished individuals are at a higher risk of developing pressure ulcers compared to normal, healthy individuals.
- Reduced skin perfusion: When blood flow to the skin is decreased, a small amount of pressure is sufficient to obstruct blood supply and cause tissue ischemia.
- Neurological diseases: Neurological disorders are associated with sensory loss and immobility. Therefore, neurological conditions like spinal cord injury, dementia, and delirium are linked with a high risk of pressure ulcer development. [6]
General Principles of Management: Pressure Ulcers
Pressure ulcers are chronic, mostly preventable wounds. For wound healing stages to progress normally, individual risk factors need to be addressed and managed. Wound care specialists should stratify the individuals at high risk of pressure development. Validated screening tools like the Braden scale, Waterlow scale, and Norton scale can be used for this purpose. Moreover, comprehensive skin assessment and examination should be done for all newly-admitted, high-risk patients.
The general principles of managing pressure ulcers is as follows:
- Optimal nutrition: Malnourishment is a contributing factor to impaired wound healing. A comprehensive assessment by a nutritionist should be carried out to address nutritional deficiencies. If oral intake is not possible, parenteral nutrition can be prescribed.
- Pain relief: Pressure ulcers are quite painful, and require effective analgesia. Pain should be graded using the "pain scale". For mild pain, simple analgesics can be prescribed. For moderate or severe pain, opioid analgesics should be considered.
- Treatment of infection: While bacterial biofilm is present in the overall chronic wounds, only clinical symptomatic infections should be treated. Cultures should be obtained, and sensitivity-guided antibiotic therapy should be initiated once culture results are available.
- Redistributing the pressure: As pressure ulcers are caused due to sustained pressure on a specific point, offloading the pressure from the site is critical in wound care. While there is no good quality evidence to suggest that regular positioning reduces the incidence of pressure ulcers, it is still recommended that position change should be done regularly in high-risk patients. [7] This should ideally be done every 2 hours.
Wound Care For Pressure Ulcers
The staging of pressure ulcers can guide the appropriate wound care strategy for pressure ulcers. For stage 1 and 2 ulcers, conservative management is applied. A transparent film is sufficient for skin protection. Surgical management is more appropriate for stage 3 and 4 ulcers.
- Periwound Skin Care: A slightly acidic pH of the skin should be maintained to avoid the risk of bacterial colonization. Skin cleansing with water and pH-neutral soaps can help maintain skin pH. Skin temperature should also be kept at an optimum level as the elevated temperature is associated with tissue damage.
- Wound Debridement: Debridement is only indicated in the presence of necrotic, ischemic tissue. Stage 1 and 2 ulcers generally do not require debridement. For stage 3 and 4 ulcers, debridement should not be done if healthy, granulation tissue is present.
- Wound Dressing: The wound dressing should be selected based on ulcer characteristics. Stage 1 ulcers have no exudate and might require no dressing. For stage 3 and 4 ulcers, however, a moisture-retaining, cavity closing dressing should be applied. For dry wounds, hydrocolloids, hydrogels, and moistened gauze are appropriate.
- Surgical Reconstruction: For extensive wounds, surgical closure of the wound should be considered. Skin flaps, musculocutaneous flaps, and skin grafts are used to surgically close the wounds. Stage 3 and 4 ulcers require surgical intervention. [8]
Patient Monitoring: How Telehealth Can Help Clinicians and Patients?
Pressure ulcers are avoidable with appropriate care and monitoring. Unfortunately, the majority of pressure ulcers occur in patients who are already bed-bound and are not able to access healthcare facilities for in-person consultations. Telehealth consultations in nursing home facilities can allow clinicians to assess the severity of pressure ulcers without the need for frequent hospital visits. Moreover, it can significantly reduce the incidence of pressure ulcers through early detection and timely interventions. [9]
References
- Reddy M, Gill SS, Rochon PA. Preventing pressure ulcers: a systematic review. Jama. 2006 Aug 23;296(8):974-84.
- Van Gilder C, Amlung S, Harrison P, et al. Results of the 2008-2009 International Pressure Ulcer Prevalence Survey and a 3-year, acute care, unit-specific analysis. Ostomy Wound Manage 2009;55(11):39-45.
- Leblebici B, Turhan N, Adam M, Akman MN. Clinical and epidemiologic evaluation of pressure ulcers in patients at a university hospital in Turkey. J Wound Ostomy Continence Nurs. 2007;34(4):407–11.
- Thomas DR. Does pressure cause pressure ulcers? An inquiry into the etiology of pressure ulcers. Journal of the American Medical Directors Association. 2010 Jul 1;11(6):397-405.
- Exton-Smith AN, Sherwin RW. The prevention of pressure sores significance of spontaneous bodily movements. The Lancet. 1961 Nov 18;278(7212):1124-6.
- Gelis A, Dupeyron A, Legros P, Benaim C, Pelissier J, Fattal C. Pressure ulcer risk factors in persons with spinal cord injury part 2: the chronic stage. Spinal cord. 2009 Sep;47(9):651-61.
- Moore ZE, Cowman S. Repositioning for treating pressure ulcers. Cochrane Database of Systematic Reviews. 2015(1).
- Anthony JP, Huntsman WT, Mathes SJ. Changing trends in the management of pelvic pressure ulcers: a 12-year review. Decubitus. 1992 May 1;5(3):44-7.
- Smith MW, Hill ML, Hopkins KL, Kiratli BJ, Cronkite RC. A modeled analysis of telehealth methods for treating pressure ulcers after spinal cord injury. International journal of telemedicine and applications. 2012 Jan 1;2012.


.webp)

.avif)