Foot ulceration is a commonly encountered complication of diabetes with a very high recurrence rate. Around 40% of people with diabetic foot ulcers will experience recurrence within one year of healing. The statistic reaches a staggering level of 65% in the next five years. [1] Patients with healed diabetic ulcers are therefore considered to be in remission instead of being regarded as fully healed. The presence of diabetic foot ulcers increases the risk of death in the next five years by about 2.5 times. [2] Therefore it is very important for podiatrists and wound care specialists to properly educate their patients about preventive strategies as these can help lower the risk of recurrence.
Why Diabetic Ulcers Are Recurrent?
Before understanding preventive strategies for diabetic foot ulcers, it is important to consider different factors that contribute to a high recurrence rate of diabetic foot ulcers. The high recurrence rate can be attributed to a combination of biological and behavioral factors. People with diabetic foot ulcers have a diminished sense of sensation due to peripheral neuropathy which is a major risk factor for unnoticed trauma. [3] Moreover, the skin is at its weakest after an ulcer has healed, which can make it more vulnerable to further trauma if appropriate protective measures are not taken. [4] In addition, patients might be under the impression that they no longer require follow-up wound care and neglect preventive measures.
Strategies to Reduce The Recurrence of Diabetic Foot Ulcers
Diabetic foot ulcers represent a significant burden to the health care system and patients. As diabetes impairs wound healing and can make wound care challenging, the recurrence of diabetic ulcers is a frequent problem due to the persistence of risk factors. The aim of an effective diabetic foot ulcer recurrence program is to improve wound healing and patients’ quality of life through early recognition and intervention. The following preventive strategies can help to reduce the recurrence of diabetic foot ulcers:
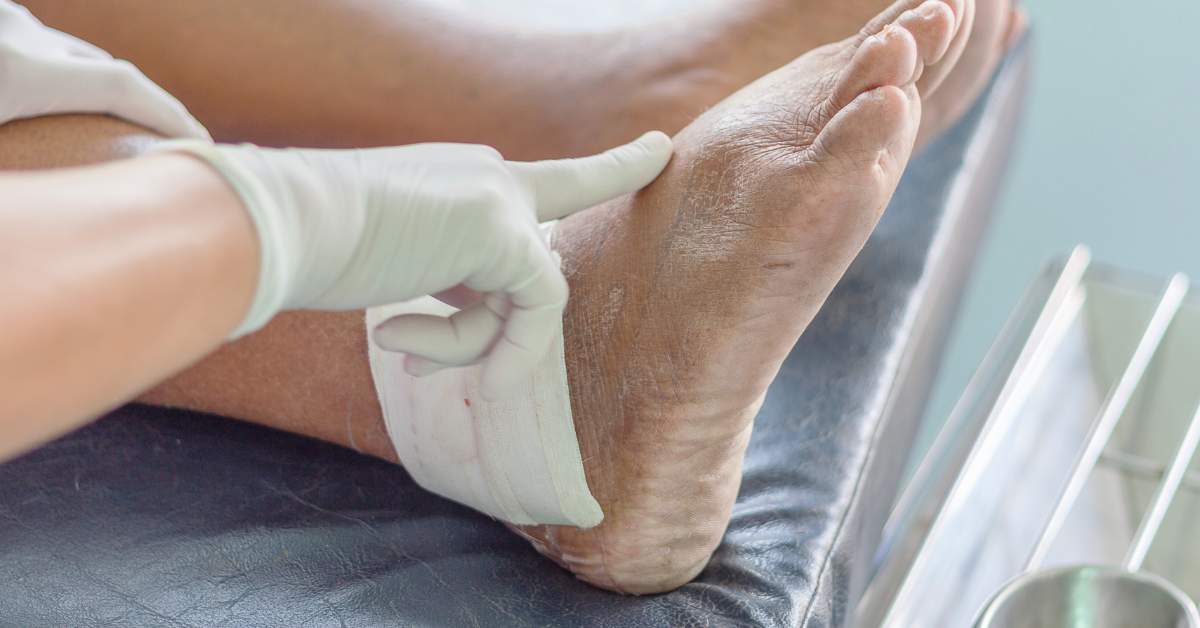
- Regular Podiatrist Visits: Regular and frequent foot examinations by podiatrists and wound care specialists is critical in the early identification of ulceration. The foot should be examined for the presence of deformities, callus formation, and early ulcerative changes. These include blister formation, fissuring of the skin, hemorrhages, and limited joint mobility. [5]
A visit to a podiatrist can also be an excellent opportunity for inspection of ill-fitting footwear that might contribute to further damage. Other factors to be considered in a foot inspection include color changes, skin temperature, foot hygiene, and fungal infections. [6] Appropriately addressing these risk factors can help in the reduction of diabetic foot ulcer recurrence. The International Working Group On Diabetic Foot (IWGDF) recommends frequent foot inspections for patients at high risk of ulceration. The visit should be scheduled once every 1 to 3 months.
- Patient And Caregiver Education: Patient education is an essential component of diabetic foot ulcer prevention. Patients need to be advised against walking barefoot as it increases the potential of foot trauma that can lead to ulceration. They should also be recommended to avoid wearing shoes without socks, shoes with thin soles, and any other type of footwear that might increase the risk of foot trauma.
Patients with diabetes are at a higher risk of excessive plantar pressure that can lead to ulceration. [7] Patients need to follow these precautions even inside their homes. Patients should be educated about the importance of regular self foot inspection and following foot hygiene. As some patients might be unable to carry out self-assessment, education should also be directed towards the patient's caregiver.
- Foot Temperature Monitoring: Patients should be informed about home skin temperature monitoring that can help in the early detection of changes that can later lead to ulceration. Home temperature monitoring combined with appropriate measures is effective in reducing the incidence of diabetic foot ulcers. These measures include patients reducing their mobility and consulting their healthcare provider after noticing temperature changes. Temperature monitoring can be an invaluable and inexpensive tool in ulcer recurrence prevention. [8]
- Wearing Protective Footwear: Patients with healed diabetic foot ulcers should always wear therapeutic, protective footwear that reduces the mechanical stress on the foot. Due to diabetic neuropathy, patients have a limited sense of sensation and require proper footwear evaluation by a trained professional. Patients can also be provided with foam to reduce callus formation and foot pressure. While custom-made therapeutic shoes might be expensive, they can be considered to be cost-effective in the long run as they have been demonstrated to reduce the incidence of diabetic ulcer risk by about 50%. [9]
- Treatment of Risk Factors: Patients should be informed about the importance of adhering to antidiabetic medication and blood sugar monitoring. Skin changes like blisters, hemorrhage and fissures are linked with increased incidence of ulceration so their early detection and treatment are important. [10] Patients should be prescribed antifungal medication in presence of fungal infections. Ingrown nails and calluses should be treated by podiatrists. Proper treatment and removal of calluses help to reduce plantar pressure which is a strong risk factor for ulcer formation. Therefore, adequately addressing and treating the risk factors of ulceration can help to reduce the recurrence rate of diabetic foot ulcers.
References:
- Armstrong DG, Boulton AJ, Bus SA. Diabetic foot ulcers and their recurrence. New England Journal of Medicine. 2017 Jun 15;376(24):2367-75.
- Walsh JW, Hoffstad OJ, Sullivan MO, Margolis DJ. Association of diabetic foot ulcer and death in a population‐based cohort from the United Kingdom. Diabetic Medicine. 2016 Nov;33(11):1493-8.
- Bus SA. Priorities in offloading the diabetic foot. Diabetes/metabolism research and reviews. 2012 Feb;28:54-9.
- Bus S, Van Netten S, Lavery L, Monteiro-Soares M, Rasmussen A, Jubiz Y, Price P. IWGDF guidance on the prevention of foot ulcers in at-risk patients with diabetes. Diabetes/metabolism research and reviews. 2016;32(S1):16-24.
- Monteiro-Soares M, Boyko EJ, Ribeiro J, Ribeiro I, Dinis-Ribeiro M. Predictive factors for diabetic foot ulceration: a systematic review. Diabetes Metab Res Rev 2012 Oct;28(7):574-600.
- Reiber GE, Vileikyte L, Boyko EJ, del Aguila M, Smith DG, Lavery LA, et al. Causal pathways for incident lowerextremity ulcers in patients with diabetes from two settings. Diabetes Care 1999 Jan;22(1):157-162.
- Fernando ME, Crowther RG, Pappas E, Lazzarini PA, Cunningham M, Sangla KS, et al. Plantar pressure in diabetic peripheral neuropathy patients with active foot ulceration, previous ulceration and no history of ulceration: a metaanalysis of observational studies. PLoS One 2014 Jun 10;9(6):e99050.
- Skafjeld A, Iversen MM, Holme I, Ribu L, Hvaal K, Kilhovd BK. A pilot study testing the feasibility of skin temperature monitoring to reduce recurrent foot ulcers in patients with diabetes--a randomized controlled trial. BMC Endocr Disord 2015 Oct 9;15:55-015-0054-x.
- Bus SA, van Netten JJ. A shift in priority in diabetic foot care and research: 75% of foot ulcers are preventable. Diabetes Metab Res Rev 2016 Jan;32 Suppl 1:195-200.
- Waaijman R, de Haart M, Arts ML, Wever D, Verlouw AJ, Nollet F, et al. Risk factors for plantar foot ulcer recurrence in neuropathic diabetic patients. Diabetes Care 2014 Jun;37(6):1697-1705.


.webp)

.avif)