Compression therapy is the gold standard treatment for patients with chronic venous insufficiency. Around 80% of all lower-extremity ulcers in the United States are caused due to chronic venous disease. Compression therapy is used in the management of venous ulcers and can include either static compression therapy or dynamic compression therapy. The results of the treatment are promising with almost 97% healing rates achieved in those compliant with compression therapy. An understanding of how compression therapy impacts wound healing is essential for wound care specialists and podiatrists.
What Is Compression Therapy?
Compression therapy is the mainstay of treatment in patients with venous disorders, lymphoedema, and thrombosis. Compression therapy involves the use of stockings or devices that provide sustained or dynamic pressure to the lower limbs. The applied pressure helps to improve the venous return which alleviates symptoms of chronic venous insufficiency. The degree of pressure applied depends on the patient's comorbid conditions, diagnosis, and the patient’s ability to withstand pressure. A pressure of 30-40 mmHg is generally sufficient to counteract the effect of capillary hydrostatic pressure in the lower limbs. Other factors that can influence the bandage pressure include calf muscle function, the shape of the leg, and the skill of the healthcare provider.
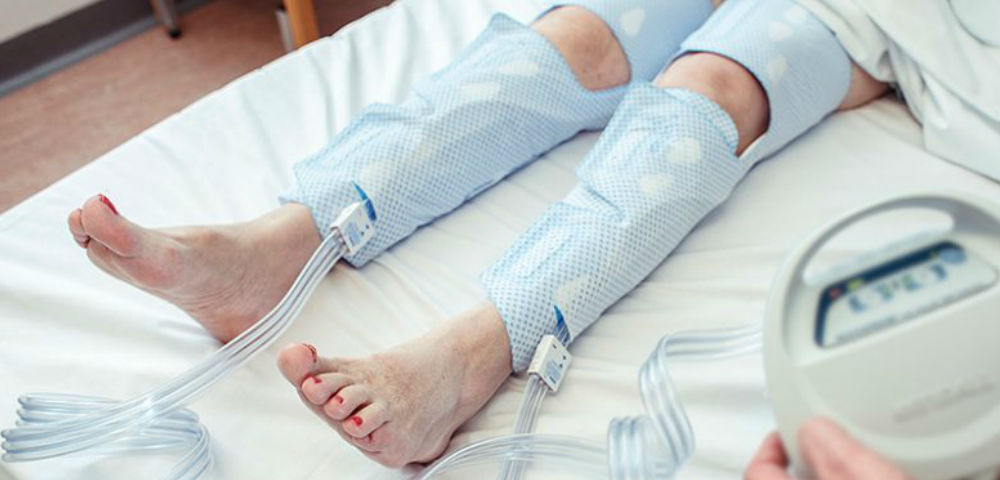
Compression therapy is not needed when the patient is immobilized and the leg is placed elevated above the heart level. Compression therapy is applied using either semi rigid dressings, Unna boots, or multi-component compression wrappings. Patients who are not able to tolerate sustained pressure might benefit from intermittent pneumatic compression therapy. It involves the use of an external pump that intermittently applies pressure to the lower limbs. It is essential that healthcare providers receive proper training before applying compression therapy. Improperly applied compression can interfere with the healing process.
How Compression Therapy Improves Wound Healing?
Properly applied compression therapy is highly successful in promoting healing in patients with venous leg ulcers. Compression therapy improves wound healing through the following mechanism:
- Increased Venous Return: As a result of sustained pressure, the vessel diameter in the lower-limbs decreases which also results in a decrease in the capillary hydrostatic pressure. In addition, compression therapy with a rigid dressing material provides stable support for the calf muscle which improves the muscle pump functioning. This consequently increases venous return which helps to reduce local edema.
- Improved Lymphatic Drainage: Chronic venous disease results in increased filtration of the capillary filtrate into the interstitium. By counteracting the capillary hydrostatic pressures, compression therapy decreases the leakage of fluid from the capillaries and also increases lymph flow. This helps to improve microcirculation at the wound site which aids in wound healing.
- Prevention Of Tissue Remodelling: The long-term application of compression therapy is linked with the prevention of tissue remodeling. This also helps to promote ulcer healing.
- Release Of Anti-inflammatory Mediators: Compression therapy has been postulated to promote the release of anti-inflammatory mediators from the endothelial cells. This in turn helps to accelerate wound healing.
- Decreased Pain: Compression therapy has been linked with decreased pain and improved quality of life in patients with venous ulcers.
Strength Of Compression Therapy During Different Phases Of Treatment
The strength of the compression therapy should be adjusted according to the patient’s symptoms and should be tailored according to therapeutic goals. It might be relevant to identify the main two phases of treatment when considering compression therapy. These include:
- Decongestion Phase: The goal of the first phase in the treatment of venous ulcers involves a reduction in local edema, and improved circulation at the wound site to aid wound healing. Therefore, a stronger compression should be applied in the initial phases of treatment. Bandages that can be used during this phase include short-stretch bandages or multicomponent systems. As wounds are heavily exudating during this phase, daily dressing changes might be needed.
- Maintenance Phase: During this phase, the main goal of treatment is to avoid ulcer recurrence and prevention of edema. As edema has usually subsided during this phase, the compression pressure applied should only be strong enough to prevent its recurrence. Higher pressure can counterintuitively result in the development of pressure ulcers. In addition, additional padding should be applied to bony structures to prevent pressure ulcer development.
Complications
Improperly applied compression therapy can result in complications. These complications are usually avoidable. Some common complications associated with compression therapy include:
- Ischemia: If the compression bandage is applied too tightly, it can compromise the blood supplying the lower limbs and result in ischemia. Signs and symptoms suggestive of ischemia include paresthesia, numbness, and discoloration of the toes. Patients are advised to seek urgent medical intervention in this scenario.
- Pressure ulcers: Pressure ulcers can develop from excessive pressure applied over the bony prominences. Therefore, additional padding to the bony points may be needed.
Contact dermatitis: Some patients could be allergic to the components used in compression bandage material. This can result in the development of contact dermatitis.


.webp)

.avif)