A venous ulcer is a common type of chronic wound that predominantly affects older individuals. It is a pathological state that results in serious physical disabilities with associated psycho-social consequences. Consequently, wound care experts must be equipped with the right knowledge and resources to accurately diagnose, and treat this serious health condition.
Defining Venous Ulcers
A venous ulcer is a chronic condition affecting the leg or foot of an individual that presents as an open lesion on the lower extremities. It is important to note that a lesion must have been present for a minimum of four months to be accurately designated as chronic.
Venous Wound Aetiology
The main causes of venous leg ulcers can be categorized into either purely venous pathologies or mixed with arterial dysfunction. Examples of causes of pure venous ulcers include reflux of the great saphenous veins in the legs and incompetence of perforator veins entering ulcer beds.
Venous ulcers of mixed origin include those caused by:
- Skin hypersensitivity
- Arterial ischemia
- Localized tissue trauma
- Lymphedema
- Wound site infection
While venous leg ulcers mostly affect the older population, younger patients with chronic venous insufficiency are also susceptible. Common factors for severe venous leg disease include obesity, diabetes mellitus, peripheral vascular disease, heart failure, obesity, and pregnancy.
Pathophysiology of Venous Leg Ulcers
The major mechanism of injury in venous leg ulcers is the onset of venous stasis. Dysfunction of the valves in veins of the lower limb results in venous hypertension as blood pools within the limbs and fails to be pumped back to the heart. This venous insufficiency results in pressure buildup within affected veins, protein loss into subcutaneous tissues, edema, and eventual tissue death from ischemia.
Clinical Signs and Symptoms
Typical symptoms of venous leg ulcers in most patients include the following:
- Pain in the affected limb(s)
- Leg cramps
- Swelling
- Itching
- Changes in appearance of affected skin (altered pigmentation, atrophie blanche, etc)
Diagnostic Procedure for Venous Ulcers
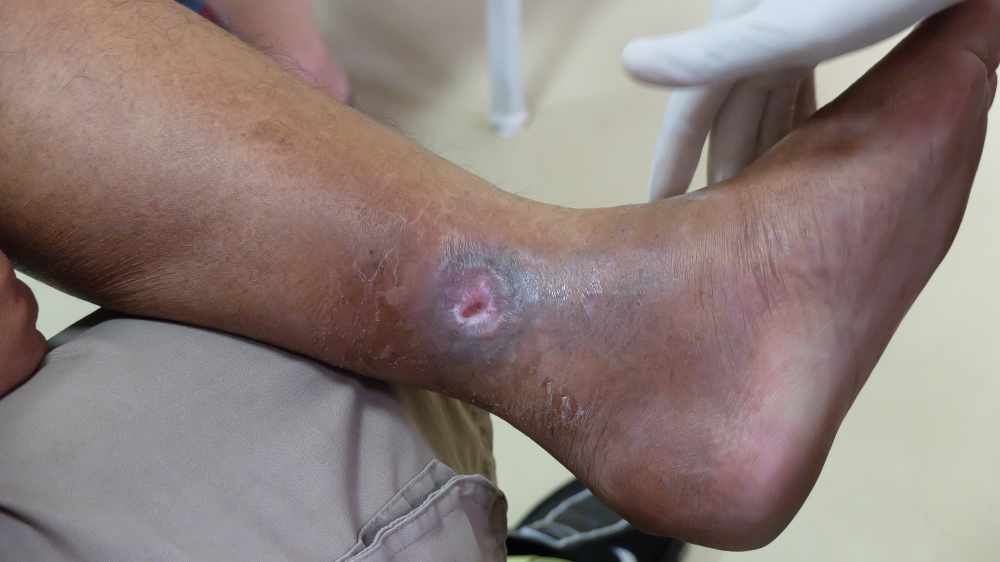
The diagnostic process for venous ulcers centers on a comprehensive physical examination. A clinical examination of the ulcer site will reveal many details to a keen observer. The most common clinical finding that supports a diagnosis of venous ulcers is the appearance of irregular, shallow ulcers with scattered fibrin and granulation tissue at the base. In addition to noticeable ulcerations over bony prominences of the legs or feet, patients with venous ulcerations might develop venous dermatitis, as well as edema and lower limb swelling. Further studies using Doppler ultrasound can be used to investigate the etiology of the ulcer and guide therapy.
Treatment Strageties for Venous Ulcers
The treatment goal in patients with venous leg ulcers is to mitigate complicating factors like tissue edema, pain, and wound site infections. Outlined below are key strategies that can be used to manage venous ulcers:
- Infection control
- Limitation of tissue edema
- Use of analgesia
- Local wound care
- Wound moisture regulation
- Surgical skin grafting
Infection Control
Judicious use of appropriate antibiotics is indicated in managing venous ulcers as they are prone to bacterial contamination, and infection. Oral or systemic antibiotics can be used to achieve microbial control within the healing ulcer sites.
Limitation of Tissue Edema
Wound care providers should counsel patients with venous ulcerations on the various methods of reducing tissue edema within, and around the ulcer sites. Patients can be given compression wear, medication, and others encouraged to perform physical exercise, and intermittently elevate their limbs.
Use of Appropriate Analgesia
The pain associated with venous ulcers can be quite significant even in patients with higher pain thresholds. As a result, wound care experts should provide appropriate and adequate analgesics to relieve this symptom. NSAIDs and opioid analgesics are viable options but drug side effect profiles must be considered.
Local Wound Care
Wound cleansing, debridement, and dressing are critical to preventing infection at the ulcer site and improving proper wound re-epithelialization. Various types of debridement can be performed including biological, autolytic, mechanical, and surgical. Removal of necrotic tissue is crucial to infection prevention. However, care must be taken when performing wound care procedures not to remove healthy granulation tissues.
Wound Moisture Regulation
Maintaining an optimal wound moisture level is another key component of venous ulcer management. Excessive drainage can be removed by the using highly absorptive wound dressing while excessive dryness can be avoided by conducting wound dressing changes as infrequently as possible.
Surgical Skin Grafting
Skin grafts gotten from donor body sites can be used to cover larger and more severe venous ulcers. This will improve their rate of healing while reducing pain, itching, and edema.
Venous Ulcer Prevention
The following strategies significantly reduce the risk of developing venous ulcers in susceptible patients:
- Use of protective footwear to avoid injury to the legs or feet
- Avoidance of prolonged periods of standing or sitting
- Cessation of harmful lifestyle choices like smoking, excessive alcohol consumption
- Avoidance of tight-fitting shoes, and pieces of clothing
- Performing regular mild to moderate physical exercises
- Routine self-examination of limbs with follow up in wound care clinics


.webp)

.avif)