Many patients with acute to chronic wounds will experience delayed wound healing due to fluid retention within damaged body tissues (edema). In some cases, the trigger for this pathological state is a dysfunction in the lymphatic system resulting in lymphedema. Due to the adverse effects of tissue edema on wound repair, wound care professionals should understand how to accurately diagnose lymphedema and provide care for affected patients.
What Is Lymphedema?
Lymphedema can be defined as the pathological accumulation of interstitial fluid within the body tissues following a compromise in the body’s lymphatic drainage system. Lymphedema can occur at birth as a congenital malformation of the lymphatic system or develop later in life when a significant obstruction to lymph flow develops. Poor circulation of interstitial fluid around the body usually results from an occlusion anywhere along the lymphatic channels leading to the accumulation of proteins outside the blood vessels. With the accumulation of protein-rich fluid within the interstitium, water is continuously pulled into the tissue spaces resulting in a physically observable swelling.
Causes of Lymphedema
Lymphedema results from damage or compromise within the lymphatic system which is present at birth or following a pathological state. The various causes of lymphedema include:
- Congenital absence/abnormality of lymph nodes or lymphatic channels
- Iatrogenic (non-intentional removal of lymph nodes during surgery)
- Malignancies (cancerous cells dislodging from tumors and blocking lymph channels)
- Obesity
- Radiation therapy
- Parasitic infestation (filariasis)
Clinical Features
Major clinical signs and symptoms associated with lymphedema are outlined below:
- Fever
- Limb swelling
- General body weakness
- Body aches
- Thickened and discolored skin
Diagnosis
Physical signs and symptoms coupled with relevant patient history and laboratory/radiological investigations are critical to the diagnostic process in lymphedema. In most cases, patients will present wound care professionals with a history of slow or rapid limb swelling. On examination, patients might have a mottled, rough, and thickened skin appearance over the affected areas in addition to obvious swelling. In some instances, signs of lymphedema will be subtle, requiring a high index of suspicion on the part of the wound care physician and appropriate radiological investigations. Imaging tests for diagnosing lymphedema include Doppler ultrasound, magnetic resonance lymphangiography, computed tomography (CT), and lymphatic radionuclide imaging.
Wound Care Strategies in Lymphedema Cases
The principles of wound care in patients with lymphedema are centered around relieving the swelling and any associated pain. Consequently, the following strategies are advised for all patients with lymphedema:
- Limb compression
- Pain control
- Massage therapy
- Daily exercise
- Total decongestive therapy
Limb Compression
Various limb compression techniques help patients with compromised lymphatic systems push static fluid out of their tissues, and relieve swelling within and around their wounds. Commonly employed limb compression techniques include:
- Application of compression with bandages
- Pneumatic compression techniques
- The use of compression wear
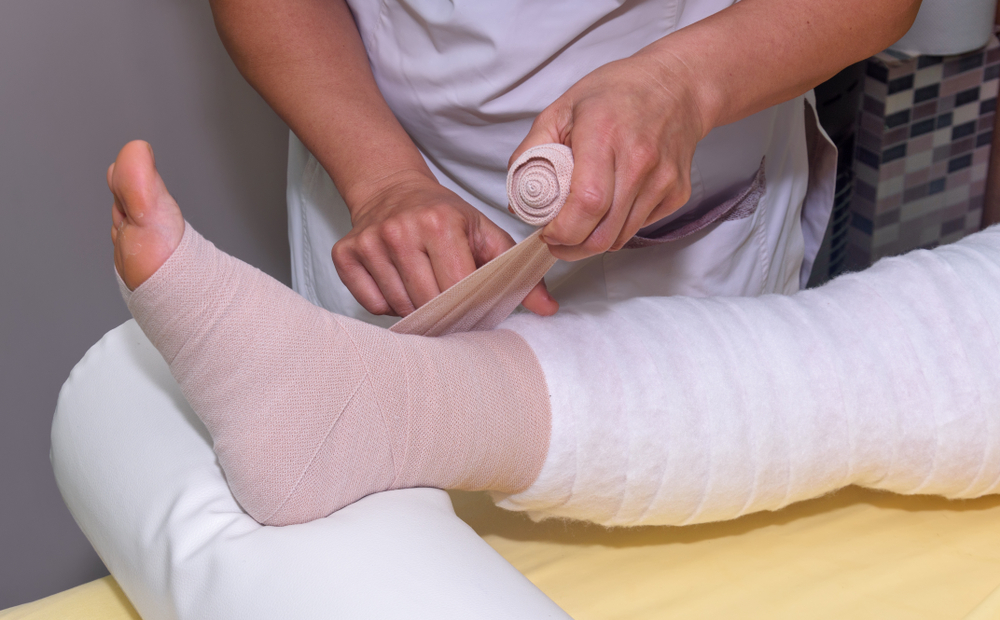
Application of Compression Bandages
Wound care experts can help facilitate the rapid reduction in the tissue swelling experienced by patients using tight compressive bandages. Bandages must fit tightly and remain secured in place to be effective in pushing excess fluid out of the wound area.
Pneumatic Compression Techniques
Automatic compression sleeves can be applied to swollen limbs to aid the movement of fluid out of the affected areas. Pneumatic pumps connected to these devices can be intermittently activated to apply physical pressure around edematous wound sites thereby draining excess fluid from the areas.
Use of Compression Clothing
These garments are typically stockings, and sleeves designed to provide continuous compressive support to a patient with edema. These specialized pieces of clothing are very beneficial in maintaining lymph fluid circulation around the body but may require the supervision of a specialist in lymphedema care to obtain the best results.
Pain Control
The pressure effects of tissue swelling can result in significant pain for a patient with lymphedema. This can lead to a rejection of wound care measures out of fear of an exacerbation of the pain. To prevent this undesirable occurrence, wound care professionals should ensure their patients receive adequate analgesia according to the severity of the discomfort reported.
Massage Therapy
Physical therapists can perform a manual lymph drainage massage for patients with lymphedema. This procedure is very effective at providing immediate relief for patients suffering pressure symptoms of lower-limb edema.
Daily Exercise
Wound care experts can encourage their patients to undergo mild to moderate daily exercises. These activities are effective at contracting muscles in the limbs resulting in improved blood, and lymph flow within them.
Total Decongestive Therapy
This approach to wound care in patients with lymphedema incorporates all the measures mentioned above, and counseling on healthy lifestyle choices. Patients should be encouraged to select an appropriate diet, minimize alcohol consumption, and quit smoking. However, patients with chronic medical conditions, such as diabetes, chronic hypertension, and cardiac disease are unsuitable for total decongestive therapy.
Prevention of Lymphedema
To minimize the risk of developing lymphedema patients with acute to chronic wounds should do the following:
- Avoid sustaining trauma to limbs by wearing protective footwear
- Allow adequate time for rest after medical or surgical treatments
- Prop the patient’s limbs on pillows above heart level for a few hours daily to allow for gravity-dependent fluid drainage
- Avoid prolonged standing in one spot
- Wear looser clothing to prevent circulatory compromise
- Keep wound sites clean at all times


.webp)

.avif)