Prolonged and excessive exposure to moisture can result in skin damage and softening which is called ‘maceration’. As excessive exudate production is a common feature of chronic wounds, maceration is an often encountered problem in wound care. Other causes of skin maceration include urinary incontinence, sweating, or leakage from a stoma. An umbrella term “Moisture Associated Skin Damage” has been recently introduced to describe the various forms of skin problems resulting from excessive moisture. Maceration resulting from chronic wound exudate is termed “periwound moisture associated dermatitis” and should be readily identified by podiatrists and wound care specialists.
How Chronic Wound Exudate Leads To Skin Maceration?
A moist wound environment is considered essential for optimal wound healing. This is because the components found in acute wound exudate accelerate wound healing through multiple mechanisms. As a result, moist wound dressings have become a standard in modern wound care. However, there is a distinction between a moist environment that is conducive to healing compared with chronic wound exudate that contains components which are detrimental to skin integrity. Therefore, it is the components of the fluid and not the fluid itself which contribute to the development of maceration.
Unlike the exudate in acute wounds, there are high levels of matrix metalloproteinases, neutrophil elastase, and other inflammatory mediators in chronic wound exudate that result in damage to the epithelium. The reduction in skin integrity predisposes chronic wounds to infections. Wound maceration has been found to delay wound healing, increase the risk of tissue necrosis, and has been associated with considerable discomfort to the patients.
Wound maceration is observed in chronic wounds such as pressure ulcers, venous ulcers, and diabetic wounds. Diabetic chronic wounds are particularly vulnerable to maceration because of neuropathic changes that affect perfusion to the skin and alter its ability to withstand trauma resulting from excessive pressure and exudate.
Identification of Wound Maceration
Wound care specialists and podiatrists need to be able to accurately distinguish between normal hydrated skin and peri-wound maceration. It is easy to mistake a newly formed epithelial tissue for maceration because of its pale white appearance. Therefore clinicians need to take clinical history and examination into consideration when suspecting a possible diagnosis of maceration.
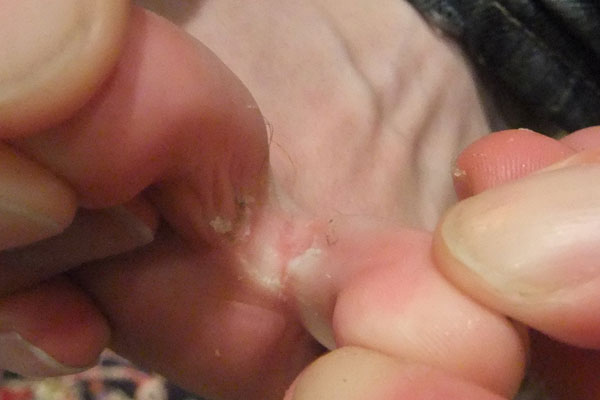
Maceration chronic wounds present with a high level of exudate and whitish, swollen skin. The surface of the skin is roughened and lined with a network of grooves termed as the “sulci cutis”. It is similar in appearance to the white, wrinkly skin observed after spending a long time in a bath. There may also be associated eczema, erythema, and necrotic tissue. In addition, there could be an extensive breakdown of the tissue in the periwound area.
Management And Prevention Of Wound Maceration
The management of wound maceration is a balancing act between excessive dryness and excessive exudate. For reduction and prevention of wound maceration, the following points should be kept in mind:
- Skin assessment and care: The periwound skin should be regularly assessed for skin damage after every dressing change. The wound edge should be properly assessed and the wound should be cleaned with normal saline.
- Selection Of Appropriate Wound Dressing: as a general rule, try to select dressing according to the level of exudate present. For wounds with heavy exudates, highly absorbent dressings such as hydrofiber, hydrocolloids, and alginates are appropriate. Regular hydrocolloid and hydropolymer are suitable for wounds with moderate exudate. For wounds with little exudate, thin hydrocolloid, and Lite hydropolymer. Occlusive dressings have the potential to exacerbate maceration and therefore should be avoided.
- Recognition and management of infection: Wound infection is linked with increased production of wound exudate. Therefore, early recognition and treatment of wound infection are essential in the prevention and management of peri-wound maceration. Silver-impregnated foam dressings have antimicrobial activity and are better in the prevention of periwound skin maceration compared to foam dressings.
- Compression Therapy: Lower-limb venous ulcers are associated with heavy exudate which can lead to maceration. Theoretically, compression therapy can help to reduce local wound exudate and edema. Therefore, compression therapy can be prescribed to patients with venous ulceration to prevent periwound skin maceration.
- Dressing Change: Wounds with heavy exudates require daily dressing change. Avoiding regular dressing changes can increase the risk of wound maceration due to excessive exposure of the wound to moisture. For wounds with a moderate amount of exudate, dressing can be kept on for five days before requiring a change. Wound care specialists and podiatrists should rely on their clinical judgment for estimation of wear time.
- Skin Protectant: Skin protectants allow the adhesive wound dressings to be applied even when the skin is damaged and allow for a wound healing environment. Studies that compared the effect of a skin protectant with a placebo for prevention of wound maceration found them to be effective. However, the barrier film was not found to be superior to zinc oxide-based protectants.
- Moisturizer: Dermatitis is a common complication of peri-wound maceration. Moisturizers can be applied to the surrounding skin to prevent the development of dermatitis. Fragrance-free formulations should be preferred especially for patients with sensitive skin.


.webp)

.avif)