The peripheral nerves are responsible for sending signals to the central nervous system (brain and spinal cord) to other parts of the human body. Peripheral neuropathy occurs due to damage to these nerves. Symptoms include numbness, muscle weakness, and a sharp, burning, or throbbing pain. Research shows that peripheral neuropathy occurs in up to 51% of patients with Type 1 or Type 2 diabetes over their lifetime. Neuropathic foot ulcers are chronic non-healing wounds that occur due to peripheral neuropathy.
Neuropathic Foot Ulcers: What They Are
Most patients that develop neuropathic ulcers have had a history of peripheral neuropathy or symptoms of vascular disease in the past, even though they might not be aware. These ulcers typically have a "punched out" shape and vary widely in size and depth between patients. They usually occur on pressure points on the foot, causing a breakdown of tissue and consequent ulceration. Risk factors for neuropathic ulcers include high blood pressure, alcoholism, hypercholesterolemia, diabetes, and a history of foot ulcerations.
Symptoms and Diagnosis of Neuropathic Ulcers
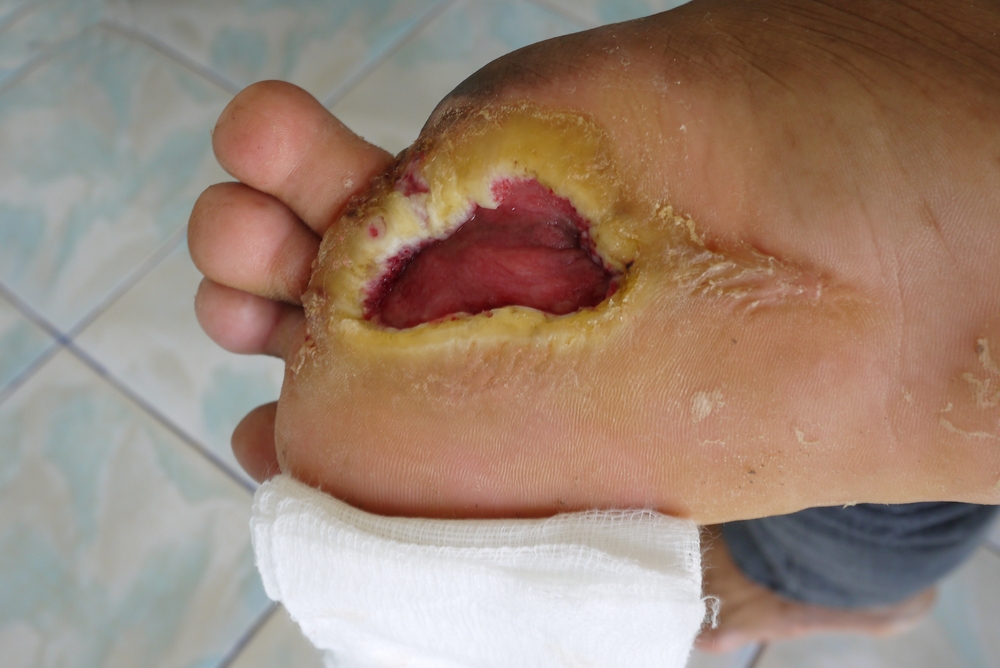
Symptoms of neuropathic ulcers may vary between patients, depending on the location and the amount of circulation. However, common clinical manifestations include calloused blisters or open sores with undermined or macerated wound edges. The depth of the wound will depend on the level of trauma to a particular area. Typically, the patient will feel no pain in the affected limb, unless there is an infection or concomitant vascular problem. Limbs will also maintain a regular pulse. Clinicians should look for signs of infection in the wound edges, as it can result in Osteomyelitis (bone infection) if left untreated. Additional signs of neuropathic ulcers include burning or tingling sensations and muscle apathy in the affected foot potentially resulting in deformities.
A review of the patient's history and a physical examination is required for a proper diagnosis of neuropathic foot ulcer. Any previous history of open wounds due to peripheral neuropathy should be noted as well as records of the patient's ankle reflex. Checking the blood glucose level of a patient in addition to serum Vitamin B12 levels may also be needed. To check for possible infection, clinicians should perform a microbiological swab test. If the patient has a history of arterial disease, the clinician should carry out an ankle-brachial index (ABI) test using a Doppler ultrasound probe. An X-ray scan may also be required in the case of Osteomyelitis.
Management and Treatment of Neuropathic Ulcers
Diabetic patients that develop neuropathic ulcers are often placed on bed rest while managing the condition. However, this approach is not ideal for most patients, as limited mobility with constant pressure on the skin often results in pressure ulcers. An alternative approach recommended by The American Diabetes Association is fitting the limb with a total contact cast (TCC) over which a small window can be cut to relieve excess pressure on the site.
Other wound management techniques include offloading, debridement, and infection control. Offloading reduces excess pressure on the wound to improve tissue perfusion in the affected foot using a or a removable cast, as previously mentioned. A podiatrist may also prescribe footwear with the proper fit to relieve pressure on the foot. Debridement removes dead or necrotic tissues and potentially infected rolled-up wound edges that may slow wound healing. Infection prevention control involves the use of topical antiseptics and antimicrobial agents to kill off bacteria.
Effective treatment of neuropathic ulcers and prevention of its recurrence may require more than classic wound care procedures. A team approach comprising a diabetes educator, podiatrist, endocrinologist, surgeon, and infectious diseases expert can be invaluable for addressing peculiarities between patients. Ongoing checks of blood glucose, and recommending dietary modifications is highly beneficial for diabetic patients.


.webp)

.avif)