Individuals at long-term care facilities are at a higher risk of developing complications from prolonged hospitalization. Pressure ulcers or pressure injuries are critical challenges faced by healthcare workers in these facilities. While prevention remains the main advocacy point, proper assessment, and therapy are crucial to improving outcomes in persons who develop pressure injuries.
What is A Pressure Injury?
A pressure injury also called bedsore, a decubitus ulcer or a pressure ulcer is an injury to the skin resulting from constant or prolonged exposure to an external force. In some cases, the force might be a constant pull subjecting the skin to tension which results in its eventual breakdown and the appearance of a defect or ulcer.
While pressure injuries might begin as a small defect, progression is usually rapidly resulting in extensive skin tissue damage within a short duration. Extension to underlying body structures will predispose an affected individual to infection which can be life-threatening if improperly handled.
Why Does A Pressure Injury Develop?
Pressure injuries are the consequences of applying a constant external force to the skin. Different types of applied force will cause varying degrees of damage depending on the duration of application.
Causes of Pressure Injury
The most common causes of pressure injuries include shear forces, unremitting skin pressure, and damage from exposure to moisture.
Shear Forces
This is quite common with patients with immobilized patients. Bed movements will cause dragging and folding of body parts which the affected individual cannot correct due to immobility. The resultant shear forces will damage internal structures while separating skin tissue.
Unremitting Pressure
Constant pressure on the skin surface will cause rapid skin damage as no recovery time is allowed for the skin to repair itself.
Moisture Exposure
Waste fluids generated by the body have corrosive effects on the skin. Fecal matter, urine, and sweat can all cause skin erosion of left in contact with it for prolonged periods.
Pressure Injuries: Who Is At Risk?
The following set of persons receiving care at long-term care facilities are at a higher risk of sustaining pressure injuries than the rest of the population:
- Individuals with prostheses as there is a risk of poor fit resulting in pressure build-up and skin damage
- People with loss of sensation from nerve damage. These individuals will not be aware of injuries sustained and ignore worsening damage
- Malnourished patients. Inadequate dietary supply of vital body nutrients is directly linked to a poor prognosis in pressure injuries
- Patients with limited mobility or total incapacitation. A detrimental pressure build-up is inevitable unless routine turning in bed is instituted
- The elderly have thinner, less resilient skin
Staging of Pressure Injuries
Pressure injury severity can be described in four stages of increasing tissue damage.
Stage 1
This is the stage of discoloration. Affected skin acquires reddish, bluish, or purple hues which stand out in stark contrast to unaffected skin. Discolored skin in the early development of pressure injuries does not blanch on physical examination.
Stage 2
Skin changes progress to the onset of superficial skin damage (blisters) in stage two pressure injuries. Typically, involvement is limited to the upper aspect of the skin (epidermis) and intervention at this point will result in a full restoration of skin integrity.
Stage 3
Stage three pressure injuries occur when the damage extends beyond the skin layers to reach the underlying sub-cut or fat layer with preservation of bone and muscle tissues.
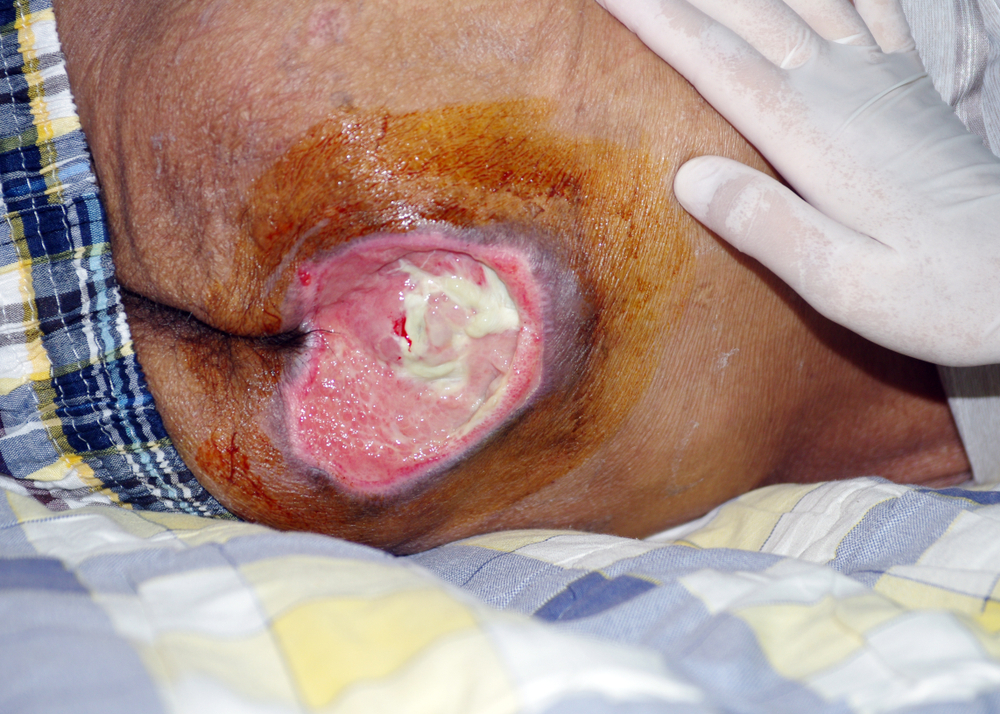
Stage 4
Ulceration reaches the bone and muscles underneath the skin. At this point, the affected individual is susceptible to life-threatening wound infections with dissemination to the bones as osteomyelitis.
Assessment of Pressure Injuries: Symptoms, Clinical Signs
Common clinical signs and symptoms that help establish a diagnosis of pressure injury are:
- Skin discoloration with non-blanching spots
- Pain/tenderness over the affected area
- Skin swelling
- Skin loss/excoriation/development of ulceration
- Discharge of purulent material from the injury site
Managing Pressure Injuries
Early intervention by healthcare providers at long-term care facilities is key to improving the prognosis for persons diagnosed with pressure injuries. The manner of therapy instituted will vary on an individual basis taking into consideration the extent of damage already present at the time of treatment.
For individuals with stage 1 and 2 pressure injuries, the treatment is mostly conservative. Regular turning in their hospital beds, the use of special mattresses, creams, ointments, improvement in nutrition, and treatment of other underlying pathologies are often enough to facilitate complete injury reversal in these cases. Gentle debridement and wound dressing have also been shown to be beneficial in stage 2 pressure injuries.
In stage 3 and 4 pressure injuries, surgery is the mainstay of treatment with flap reconstruction to restore skin cover. Wound reconstruction in patients with advanced-stage pressure injuries is a delicate procedure with high complication rates. These corrective procedures should be performed by experienced, high volume surgeons only after adequate infection control has been attained. Post-operative monitoring is equally as critical to ensure a good overall outcome with wound care, optimal nutrition and antibiotic therapy all play key roles.
Apart from conservative medical therapy and surgery, other treatment options with unproven effectiveness currently undergoing research are hyperbaric oxygen therapy, recombinant growth factor use, negative pressure wound therapy (NWPT), and electrotherapy.


.webp)

.avif)