Bacteria first appeared 3 billion years ago and have been associated with considerable morbidity and mortality in humans. Before the discovery of antibiotics, bacterial infections were the leading cause of human death. Diphtheria, cholera, Bubonic plague, and countless other bacterial diseases wreaked havoc on humanity for hundreds of years. With the discovery of penicillin began the golden age of medical science. Bacterial diseases were expected to become a thing of the past but they didn't. With the indiscriminate use of antibiotics came a much bigger problem that grows larger with each passing day: drug resistance.
What Is MRSA?
Staphylococcus Aureus is a type of Staphylococcus bacteria. It is a gram-positive facultative aerobe that forms golden colonies on culture. It is found in the environment as well as the human body. It colonizes the skin and mucous membranes of healthy individuals. However, it can cause a variety of clinical diseases if it enters the bloodstream. After Staphylococcus Aureus developed resistance to penicillin only a few short years after its discovery, a new drug was introduced in the late 1950s: methicillin.
Methicillin is a penicillinase-resistant penicillin that was created to counter the effects of penicillin resistance. Unfortunately, the bacterium evolved again and underwent mutations that made it resistant to the effects of methicillin. The new resistant strain was called Methicillin Resistant Staphylococcus Aureus or MRSA. Initially thought of as a hospital-acquired organism, MRSA spread to the community and to date plays a major role in resistant/recurrent bacterial infections.
MRSA and Chronic Wounds
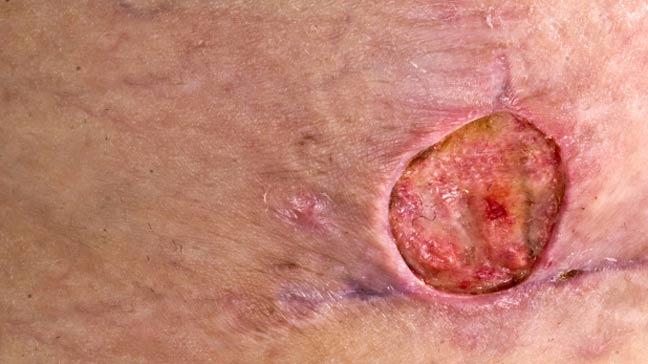
A chronic wound is defined as a breach in the skin or mucous membrane that does not heal in a timely fashion. Some sources give a timeline of three months before classifying a wound as ‘chronic’. Examples of chronic wounds include pressure ulcers, venous ulcers, diabetic ulcers, infected surgical or traumatic wounds, etc. The etiology usually involves decreased blood flow, neuropathy, infection, systemic illness, comorbidities, and advanced patient age.
Chronic wounds result in a disruption of the dermal barrier providing an entry point for microorganisms. This loss of barrier function coupled with prolonged inflammation makes chronic wounds susceptible to superadded infections. Most chronic wound infections are polymicrobial and multiple organisms work together to establish a protective biofilm. The biofilm aids and nourishes the microorganisms and causes further delay in healing. Staphylococcus aureus, Pseudomonas aeruginosa, E Coli, and Proteus mirabilis are among the most common pathogens isolated from infected chronic wounds. While MRSA is not the most common microorganism in chronic wound infections, its prevalence is increasing day by day.
Despite forming a comparatively small percentage of chronic wound infections, MRSA is a major obstacle in wound care as it is difficult to treat and leads to worse outcomes. It is associated with a greater risk of bacteremia and poses a significant healthcare burden.
Tetracyte - A One of a Kind First Aid Topical Antibiotic
Tetracyte is an FDA-approved broad-spectrum topical product marketed by WoundPros LLC. Created with decades worth of experience by top professionals, Tetracyte combines powerful ingredients with state-of-the-art Dual Carrier Technology (DCT).
The active ingredient is Tetracycline Hydrochloride 3%, a potent broad-spectrum antibiotic effective against gram-positive bacteria, gram-negative bacteria, and atypical organisms.
What sets Tetracyte apart? Not only is it effective against a wide range of susceptible strains, but it also boasts an impressive kill rate against resistant strains like MRSA and MuRSA.
Using Tetracyte for MRSA-Infected Chronic Wounds
Tetracyte is a successful treatment option for superficially infected chronic wounds. It has a greater than 99% kill rate for common chronic wound pathogens like Staphylococcus Aureus, Pseudomonas Aeruginosa, and Eschericia Coli. More importantly, it has a 99.65% kill rate against MRSA. Clinical trials show Tetracyte to be effective even in chronic MRSA-infected wounds resistant to intravenous Vancomycin. Going a step further, it also has a 99.57% efficacy rate against MuRSA.
Mupirocin is an antibiotic used to treat resistant strains of Staphylococcus Aureus. However, MRSA is becoming increasingly resistant to the bactericidal effects of Mupirocin resulting in a new threat: Mupirocin Resistant Staphylococcus Aureus (MurSA). Tetracyte counters this problem effectively and affordably.
Clinical studies show that Tetracyte is potent, fast acting, and has minimal side effects. The Dual Carrier Technology ensures maximum penetration of bacterial cell walls combined with a strong desiccant effect. The only side effect is mild localized irritation. Unlike Mupirocin which carries the risk of anaphylaxis, rash, and urticaria, Tetracyte is not absorbed into the bloodstream and the risk of systemic toxicity is negligible. Patients report visible improvement in symptoms within 24 hours of application with complete resolution in a few weeks.
Tetracyte is not only a powerful antimicrobial agent, but it is also enriched with a cocktail of healing ingredients like Dimethyl sulfoxide (DMSO), Cholecalciferol (Vitamin D3), and Ascorbic Acid (Vitamin C). These compounds have intense regenerative and antioxidant properties resulting in faster healing, enhanced vascularisation, and improved general skin condition.


.webp)

.avif)