Healthcare providers universally agree that an increasing burn severity is associated with a poorer prognosis. Full-thickness burns fall into this category of serious, life-threatening burns with dire outcomes. Although a complete restoration of structure and function is not a realistic goal in managing full-thickness burns, early diagnosis and comprehensive treatment should seek to limit post-repair sequelae.
What Constitutes a Full-Thickness Burn?
Full-thickness burns involve the reticular dermis and hypodermis respectively. The damage associated with full-thickness burns is quite significant because the entire thickness of the skin is affected with burns reaching the underlying subcutaneous tissues.
Etiology/Risk Factors
Burn wound etiology is broadly classified into six groups/exposures:
- Scalds
- Contact burns
- Direct flame exposure
- Electrical
- Chemical
- Radiation
With exposure to hazardous materials and environments, any member of the population can be affected by full-thickness burns. However, adults within the working-class population are more likely to sustain full-thickness burns. The groups predominantly at risk factors for developing full thickness include:
- Females due to a slightly higher exposure to open flames
- Unsupervised children within high thermal-risk domestic environments
- Elderly persons due to lower sensory perceptions within potential burn environments
- Workplace exposure (metalworkers, chemical manufacturing, oil and gas production, and food workers)
Full Thickness Burns: The Clinical Picture
Full-thickness burns present with the following signs and symptoms:
- A charred or pale and leathery appearance of skin over the affected area
- Increased moisture of burned skin area
- Loss of pain sensation due to nerve damage from severe burns
Diagnosing Full Thickness Burns
Diagnosis of full-thickness burns can be done using a combination of physical examinations and burn wound assessment charts. The presence of clinical signs such as a failure to elicit a pain response from the burn site as well as visible signs of complete damage to the entire skin is key pointers to a full-thickness burn. Further, an assessment of the burn depth and severity are also integral to correctly diagnosing a full-thickness burn.
Similar to assessments done for a partial-thickness burn, severity estimation can be done using the Lund and Browder chart, palmar surface estimation, or very commonly the Rule of Nines. Depth categorization can be done clinically by surgeons or with the aid of laser Doppler technology with the latter providing more accurate estimations.
Treatment Approaches
A full-thickness burn is a serious event with dire hemodynamic and physiological consequences on the affected individual. All treatment approaches must try to revert or control the instabilities resulting from a burn of this severity.
The key treatment strategies crucial to successfully stabilizing a patient with full-thickness burns are outlined below:
- Fluid therapy
- Wound care
- Oxygen therapy
- Tetanus prophylaxis
- Infection control
- Surgery
- Pain control
- Rehabilitation
- Counseling and psychological support
Fluid Therapy
Full-thickness burns predispose affected patients to severe dehydration due to increased fluid losses from damaged skin. Left unchecked, fluid losses will cause hemodynamic instability and tilt the patient into clinical shock. Early institution of intravenous fluid therapy with Normal Saline or Hartmann’s Solution will prevent the onset of dehydration and its sequelae while improving the patient’s clinical state.
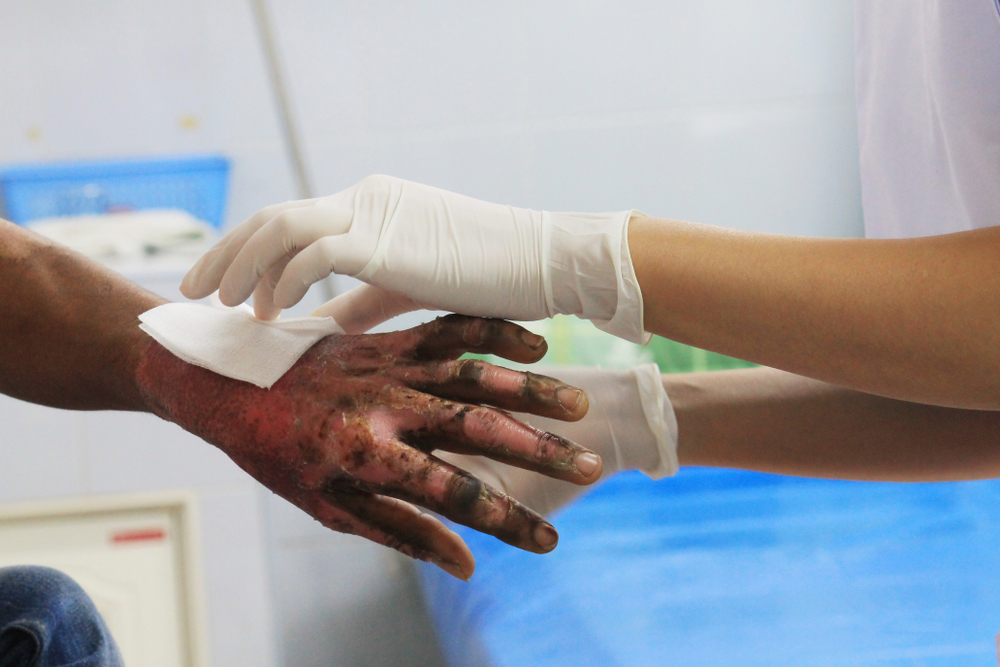
Wound Care
Patients with full-thickness burns require diligent wound care at all stages of healing. Adequate wound cleaning, dressing, debridement (removal of devitalized/dead skin tissue), and eschar removal, are all required to promote wound re-epithelialization and optimize the healing process.
Oxygen Therapy
In some cases, full-thickness burns such as those affecting the face and neck, are associated with inhalation injuries which can be life-threatening. In these cases, the use of oxygen support therapy is indicated.
Tetanus Prophylaxis
Tetanus prophylaxis should be instituted in all full-thickness burn patients to eliminate the risk of developing the fatal disease.
Infection Control
Prophylactic and therapeutic antibiotics are an integral part of wound care in full-thickness burns. These medications prevent the onset of infection or limit its spread if already present. The type of antibiotic/route of administration will vary between patients based on burn severity, local bacterial resistance patterns, and clinical status. Topical, oral, and intravenous preparations can all be used in managing full-thickness burns.
Surgery
As a general rule, full-thickness burns require some form of corrective surgery at a later point in the management process. Reconstructive surgery with skin grafting can be used to minimize the effects of extensive scarring associated with this type of burn.
Pain Control
Although the initial period following a full-thickness burn is associated with diminished or complete lack of pain sensation over the burn area, analgesics will be needed to treat chronic pain which may develop over time.
Rehabilitation
Physical and occupational rehabilitation are crucial aspects of treating full-thickness burns. Physical and occupational therapies will help affected individuals regain as much range of limb function as possible and prepare them for reintegration into their home and work activities after discharge from the hospital.
Counseling and Psycho-social Support
Sustaining a burn injury can be an emotionally traumatic experience regardless of severity however, the psychological component is more profound in severe burns. Patients with full-thickness burns should be provided with adequate professional counseling and psycho-social support to help them through the physical recovery process and life afterward.


.webp)

.avif)