An imbalance in certain physiological and biochemical aspects of chronic wound healing can result in various complications including wound infection spreading to the bones as osteomyelitis. In this article, we will outline the risk factors responsible for this serious complication and also establish the appropriate treatment procedures required to correct it.
What is Osteomyelitis?
Osteomyelitis is inflammation of the bone due to infection with pathogenic microorganisms. While the bone is typically impermeable to bacterial colonization, disease-causing microbes can gain access to the bone via the bloodstream following bacteremia, trauma cause bone fractures, surgical procedures, such as the placement of prostheses and iatrogenic introduction of infected foreign bodies to bony cavities.
Most cases of osteomyelitis are caused by the bacteria Staphylococcus aureus however, other causative bacteria have been isolated from patients confirmed to have the disease. The causative organism usually varies with age as distinct subsets of the population are more susceptible to diverse bacterial pathogens.
Etiology/Risk Factors for Osteomyelitis
The primary cause of osteomyelitis in a person with a chronic wound is hematogenous spread from the wound site through the bloodstream to the bones. The blood vessels supplying the bones can conduct pathogens that settle within them causing destructive changes in bone structure.
Secondary causes of/risk factors for the development of osteomyelitis include:
- Poor asepsis during surgical procedures
- Accidental traumas causing bone breaches/fractures
- Sepsis
- Smoking
- Chronic medical conditions (diabetes mellitus, kidney disease)
What Symptoms or Signs Suggest Osteomyelitis in Chronic Wounds?
Poor healing, chronic wounds are highly susceptible to the development of wound site bacterial colonization, and subsequent dissemination to nearby bones. While the clinical picture will vary, patients will often complain of the following symptoms:
- Fever
- Swelling over bones
- Pain
- A general feeling of being unwell
A clinical examination by a physician may elicit one or all of the following signs:
- Moderate to high fevers
- Chills
- Tenderness and swelling over bones
- Differential warmth of skin overlying affected area
Unfortunately, some cases of osteomyelitis might have vague symptoms or no symptoms at all. In these cases, without a high level of suspicion by the clinician in charge of the case, and prompt confirmation with the help of imaging modalities like X-rays and CT scans, early intervention might be delayed resulting in less optimal outcomes.
Pathophysiology of Osteomyelitis in Chronic Wounds
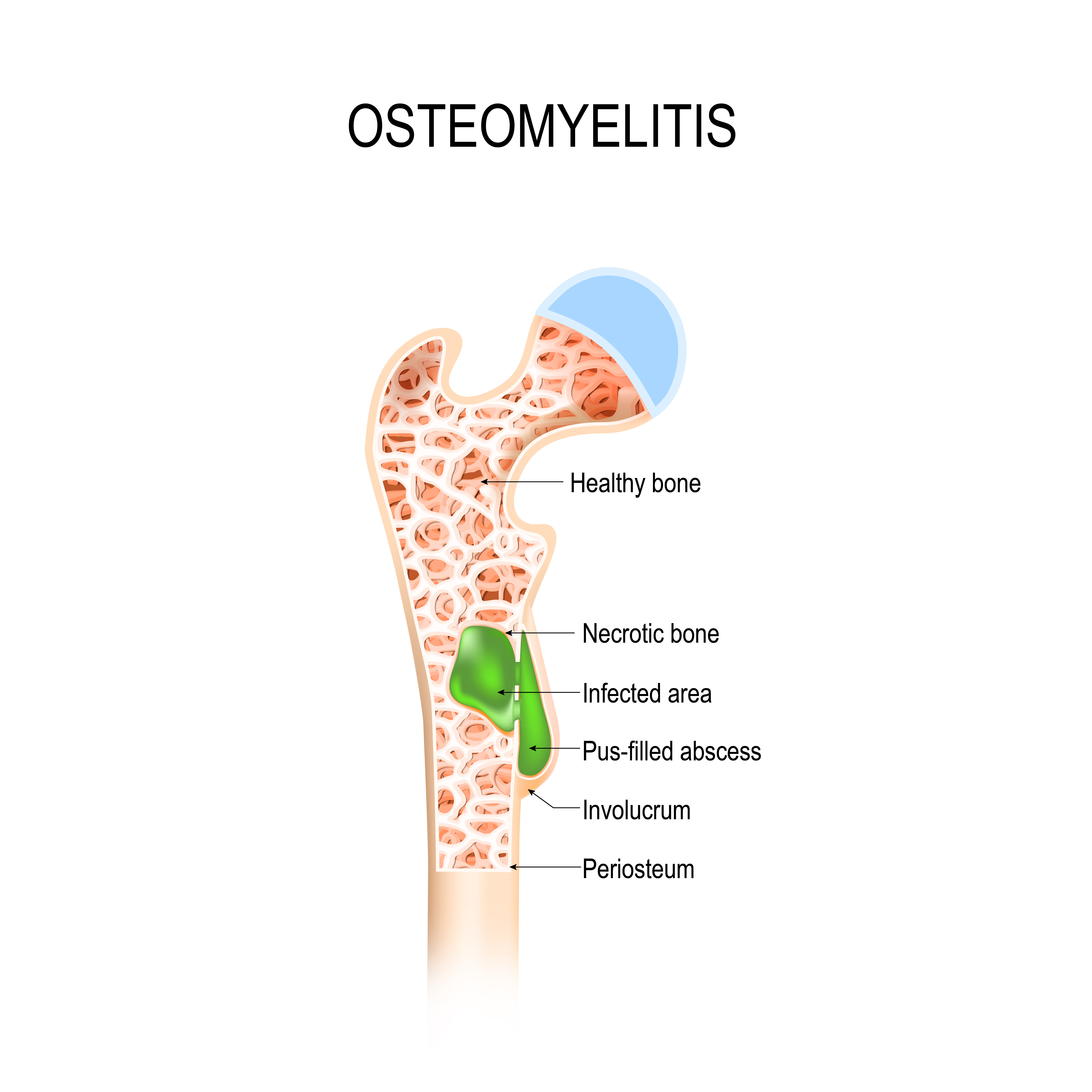
Bone involvement in osteomyelitis results from bacterial dissemination from a chronic wound or new trauma to the wound site. Bacteria inoculation can occur in virtually any bone but most commonly occurs in bones in the lower limbs. Diabetic foot ulcers and wounds resulting from a peripheral arterial disease commonly display dissemination to the long bones in the lower limbs (femurs) and the pelvic bones. Bacteria colonization within these bones compromises blood supply leading to ischemia and necrotic bone damage. The body attempts a physiological repair response leading to the formation of new bone mixed with dead or dying bone resulting in structural deformities.
Treatment Strategies for Osteomyelitis in Patients with Chronic Wounds
An effective treatment approach to osteomyelitis in a patient with a chronic wound requires the cooperation and communication of a team of specialists including physicians (infectious disease specialists), surgeons (plastics and orthopedics), microbiologists, nursing care practitioners, physiotherapists, and other support staff.
Key treatment strategies include:
- Local wound care
- Medical therapy
- Surgical interventions
Local Wound Care
Facility or home-based nursing care is required to minimize bacterial colonization worsening outcomes in individuals with chronic wounds complicated by osteomyelitis. Wound debridement with removal of de-vascularized tissues, routine wound dressings with saline and other dressing materials, and foreign body removal are all crucial aspects of nursing wound care. When done properly, these actions will limit bacterial growth, and inflammation allowing an early halt in destructive processes in affected bones.
Medical Therapy
Medical treatments for osteomyelitis revolve around the safe and rational use of antibiotics. An evidence-based approach is to prescribe antibiotics with proven activity against organisms cultured from a wound site. Wound swab culture and sensitivity tests will help guide antibiotic administration. Depending on the severity of infection, antibiotic therapy can be stepped up from standard classes to highly potent drug types. Common antibiotic classes used in drug therapy for osteomyelitis include fluoroquinolones, penicillins, and sulphadrugs.
Surgical Interventions
Extensive damage to bone structures resulting from osteomyelitis will require corrective surgeries in most instances. Surgical debridement, fixation of traumatic or pathological fractures, and correction of deformities are components of the surgical response to osteomyelitis in chronic wound patients. In an individual with dead spaces due to bone loss, the use of surgically implanted antibiotic materials can serve as a temporary measure till definitive procedures are possible. Other surgical techniques include the Ilizarov technique, wound closure, and adjunctive hyperbaric oxygen therapy.
Prevention
The prevention strategies for osteomyelitis involves proper counseling of persons with chronic wounds about the risk factors for its development and the need for strict adherence with wound care/infection control. Patients should be counseled to quit harmful lifestyle habits like smoking, invest in exercising/dietary control, perform their role in wound care, and comply with the use of prescribed medications.


.webp)

.avif)