An optimal wound microenvironment is essential for wound healing. The work of George Winter (1960) highlighted the importance of a moist wound environment for best healing outcomes. Before his work, it was historically assumed that wounds heal better if left open in the environment. As a result, a variety of wound dressings have been developed since then that play an active role in the wound healing process. Hydrocolloid wound dressings are amongst the earliest wound dressings developed that were able to optimize moisture in the wound microenvironment. Podiatrists and wound care specialists need to be aware of the indications for these types of dressings.
Hydrocolloid Wound Dressings: An Overview
Hydrocolloid wound dressings were first introduced in wound care during the 1980s and quickly became one of the most widely used wound dressings. These dressings have two layers: an inner colloidal layer and an outer impermeable layer. Hydrocolloid wound dressings are composed of a combination of gel-forming substances that in the presence of wound exudate, cross-react to form a gel. Some of the substances in the composition of hydrocolloid dressings include pectin, absorbent polymers, and sodium carboxymethylcellulose.
Early forms of hydrocolloids used to be fully occlusive. However, recent hydrocolloid dressings tend to be 'semi-occlusive'. This means that they are impermeable to bacteria and larger molecules but permeable to water vapors. This makes them excellent in retaining moisture in the wound bed which is essential for wound healing.
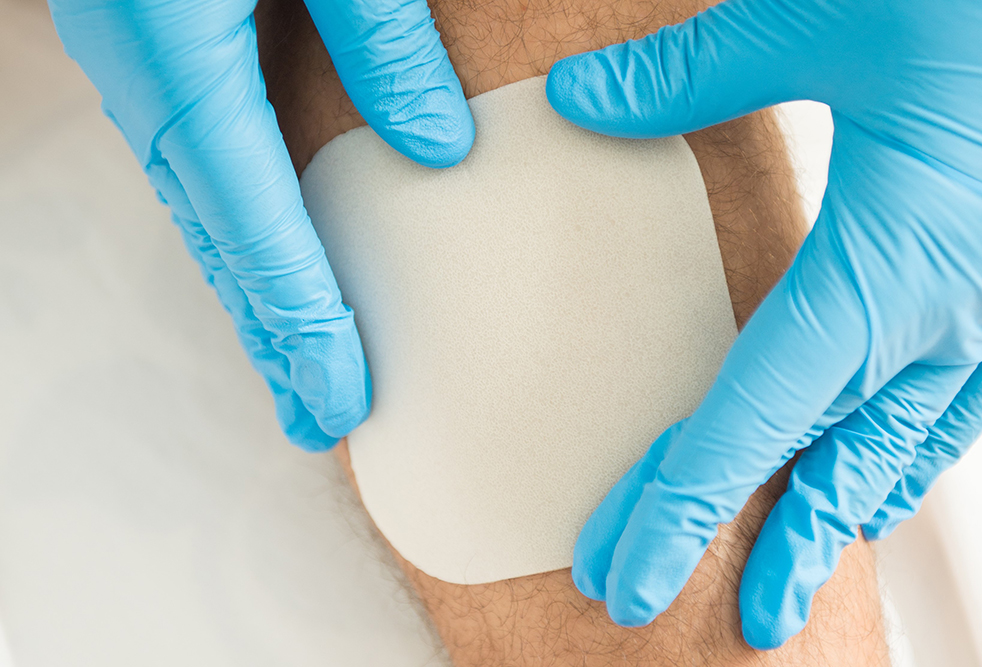
Hydrocolloid dressings are available as wafer-shaped dressings in several shapes and sizes. They are also available as ‘contoured dressings’ that make them suitable for use at anatomically challenging locations. Even though they are mostly used as primary dressings, hydrocolloid dressings can function as secondary dressings in conjunction with alginates and hydrocolloid pastes. Examples of commonly available hydrocolloid dressings include Granuflex, Tegasorb, and Comfeel.
Benefits Of Hydrocolloid Dressings
Hydrocolloid dressings represent the modern advancement in wound care. Unlike traditional wound dressings that had a passive role in wound healing, modern wound dressings actively stimulate wound healing due to their special characteristics. Some of the benefits of hydrocolloid wound dressings include:
- Moist wound environment: On exposure to the wound exudate, hydrocolloid dressings form a gel-like substance that can maintain wound moisture. As a moist wound environment is crucial for wound healing, hydrocolloid dressings can improve healing outcomes.
- Decreased risk of infection: The gel-like substance that is formed by hydrocolloid dressings can trap bacteria and other contaminants. In addition, some hydrocolloid dressings lower the wound pH which makes them ideal for reducing the risk of wound infection.
- Easy monitoring of wound: Hydrocolloid dressings are translucent in appearance which allows podiatrists and wound care specialists to better assess and monitor the wound. The wound fluid and its appearance can also be observed underneath the dressing.
- Autolytic debridement: Autolytic debridement is the removal of devitalized necrotic tissue by the body's enzymatic system. By allowing for the accumulation of wound exudate at the wound site, hydrocolloid dressings facilitate autolytic debridement.
- Fit inaccessible locations: Hydrocolloid dressings come in a variety of shapes and sizes. In addition, they also contour well which makes them suitable for use at inaccessible locations.
- Protection of skin: Hydrocolloid dressings protect skin from friction and external trauma.
Indications For Hydrocolloid Dressings
Hydrocolloid dressings do not have a good absorptive capacity which makes them appropriate for wounds with moderate to minimal exudate. Some of the indications for hydrocolloid wound dressings include:
- Abrasions
- Skin tears
- Lacerations
- Wounds with moderate to minimal exudate
- Pressure ulcers
- Dermal wounds
- Necrotic wounds
- Partial and full-thickness wounds
- Surgical wounds
- Preventive dressings: sacrum, heels
Newer hydrocolloid dressings have better absorptive capacity and might be used for wounds with moderate to heavy exudate.
Important Considerations
Some important considerations need to be taken into account while using hydrocolloid dressings. These include:
- Hydrocolloid dressings should be changed within 3-7 days as prolonged use is associated with maceration of periwound skin.
- Hydrocolloid dressings should be used over sinus tracts or tunnels
- Not all hydrocolloid dressings are suitable for infected wounds so product labels should be carefully read before use.
- Hydrocolloid dressings might be associated with malodor which is especially noticeable during dressing changes. In the absence of clinical signs of infection, this is usually considered to be normal.
- Hydrocolloid dressings should be used with care on fragile skin due to their adhesive property.


.webp)

.avif)