Like other dermatological disorders, lower limb cellulitis accounts for an unsustainable number of hospital admissions in the US annually, placing further strain on limited healthcare resources. However, due to limited awareness of the condition, many cases go undiagnosed and progress into severe infections with life-threatening implications. This article will discuss the symptoms, diagnosis, and treatment options for cellulitis of the lower extremities.
What is Lower Limb Cellulitis?
Cellulitis is a medical condition that occurs due to bacterial infection of the skin. Affected skin may appear swollen, reddish (erythema), tender, and warmer than surrounding areas, and infection can spread rapidly if left untreated. In severe cases, even it can progress into subcutaneous tissues, bloodstream, lymph nodes, and vital organs, which can result in death. Cellulitis can occur in any part of the body; however, it commonly affects parts of or the entire lower legs, particularly the ankles and shins. Cellulitis is either wet or dry. Dry cellulitis is more common, with erythema that spread over large areas causing tissue damage, but no blisters. The wet type, on the other hand, produces blisters from time to time.
What Causes Lower Limb Cellulitis?
Bacteria can be introduced into a wound through cuts, abrasions, bruises, venous eczema sites, or areas without skin, e.g., in tinea pedis (athlete's foot). Common cellulitis pathogens include Group A ß - Hemolytic streptococcus, Streptococcus pneumoniae, and Staphylococcus aureus. Although these bacteria are normally present in mucous tissues of the nose and mouth in healthy people, they can cause severe infection in open wounds.
Diagnosis
Diagnosing cellulitis should be done based on a patient's medical history and a physical assessment. Samples of the blood and skin can be vital for determining the causative bacteria. Although timely diagnosis and intervention are vital, diagnosis of lower limb cellulitis can be challenging for the following reasons:
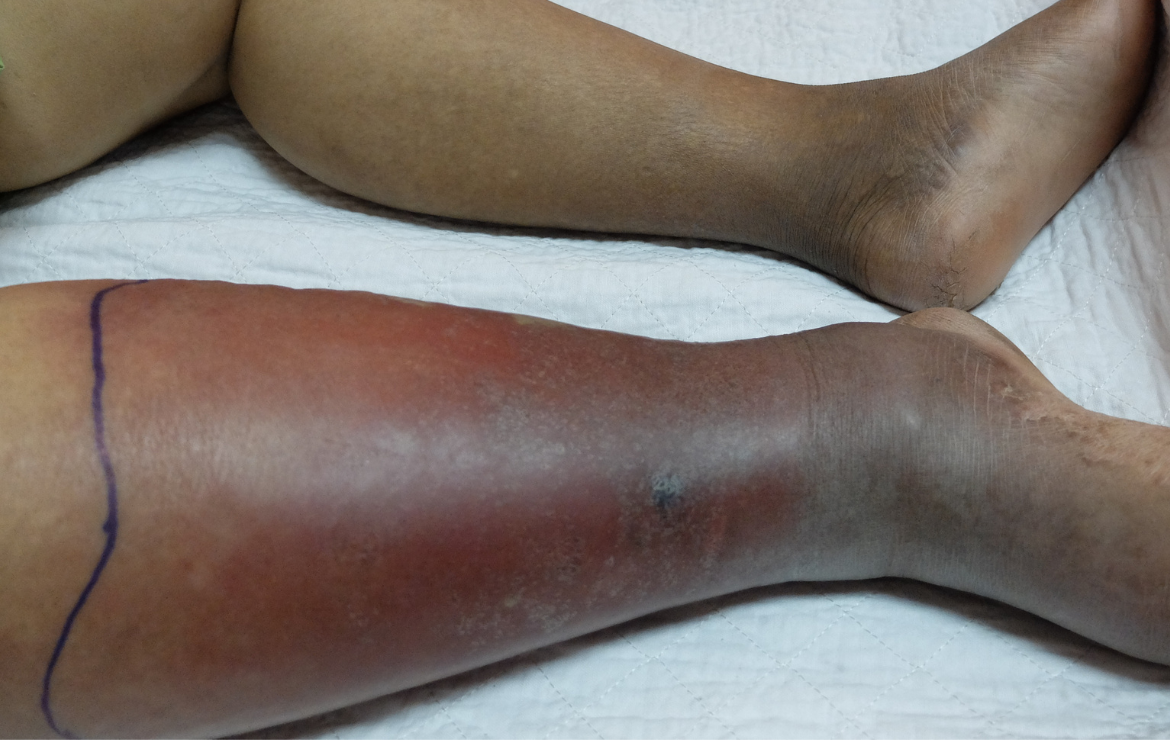
- Dark skin can mask erythema (redness of the skin and cellulitis demarcation lines are less visible in people of color)
- Inflammation due to cellulitis may be confused with symptoms of venous or arterial disease (the presence of infected venous ulcers and undiagnosed tinea pedis can result in misdiagnosis).
Distinctive symptoms of cellulitis include skin tenderness and erythema with an observable difference in temperature to the surrounding skin. These symptoms may be accompanied by a fever or malaise. Other symptoms include maceration and acute pain in the affected areas.
Risk Factors
There is a wide range of risk factors for developing cellulitis. Possible causes include:
- Leg or foot ulcerations in diabetic patients
- Skin injuries due to trauma (e.g., abrasions, cuts, and bruises) or surgical wounds that become infected
- Obesity
- Liver diseases, such as cirrhosis or chronic hepatitis
- Edema due to poor circulation
- Contaminated foreign objects inside the skin (e.g., intravenous catheters and other surgical equipment)
- Recurring skin lesions due to chronic skin disorders, such as psoriasis or eczema
- Bites and stings from humans and certain animals
- Fungal infection in the limbs and toes, such as tinea pedis (athlete's foot) or contact dermatitis.
Treatment of Cellulitis
After the initial assessment and diagnosis, cellulitis can be treated using antibiotic therapy. A combination of benzylpenicillin and flucloxacillin is often used. The effectiveness of the therapy, however, will depend on whether the patient has wet or dry cellulitis. Wet cellulitis may require a wound swab to determine the pathogen and its sensitivity to antibiotics. Antibiotics for cellulitis can be administered orally, through injections, or intravenously. In severe cases of cellulitis with extensive tissue damage, surgery will be required to drain abscess or remove necrotic tissue.
According to a study published in the New England Journal of Medicine, compression therapy may be a viable technique for preventing the recurrence of lower limb cellulitis. However, clinical evidence to support its effectiveness is currently sparse. Compression bandaging can help to relieve chronic edema and is only used as an adjunctive therapy. Limb elevation and exercise can also help to reduce venous pressure in the affected limb(s). Effective management of cellulitis involves regular assessments of skin integrity and the use of topical antiseptics and dressings to manage any associated skin diseases that contribute to its recurrence. Clinicians must also keep the affected areas clean and dry and ensure the patient gets enough rest to improve the recovery period.


.webp)

.avif)