Depending on the nature and severity of sustained wounds, treatment protocols will vary. While less severe injuries can often be treated at home using first aid kits, most chronic wounds require expert care that can only be provided by competent and licensed professionals. In these cases, wound management is based on industry best practices or principles targeted at complete wound repair with minimal post-healing complications.
Wound Management: Aims and Objectives
Every wound management principle is implemented for one or more of the following aims:
- To eliminate dead tissues and preserve healthy/viable tissues
- Achievement of proper re-epithelialization and wound closure
- Reduction/elimination of wound tissue inflammation
- Infection prevention/control in the wound area
Wound Management Principles for Professionals
A more advanced understanding of human anatomy and associated physiological body processes allow healthcare professionals to provide more optimized care than is possible with non-trained caregivers. Healthcare staff follow certain principles based on their understanding of the human body to provide the possible conditions for proper wound healing to take place.
Key universally recognized wound management principles include the following:
- Hemostasis
- Wound classification
- Assessment/modification of risk factors
- Infection control
- Wound cleaning and debridement and dressing
- Oxygenation and moisture control in the wound environment
- Appropriate analgesia
- Skin wound closure
- Nutritional support
- Adjunct therapy
Hemostasis
The initial first step in wound management is securing hemostasis (stoppage of bleeding from an injury). With any breach in the skin surface, some degree of bleeding is expected and it is critical this is stopped before any further intervention. While hemostasis occurs spontaneously in most cases, techniques like pressure application, limb elevation, suturing, and the use of tourniquets might be required to staunch bleeding in more severe wounds.
Wound Classification
Another essential step in achieving satisfactory wound repair is determining the type of wound involved. Wounds can be broadly divided into five categories based on the mechanism of injury: avulsion, abrasion, puncture, laceration, and incisions. Wound classification based on duration is of two types; acute and chronic. Acute wounds usually disappear after a few weeks while chronic wounds take a longer time to heal typically months to years. In each of these cases, further steps in management will differ greatly.
Assessment/Modification of Risk Factors
Each patient presenting to a healthcare provider must undergo screening for risks associated with the poor wound healing progress. Risk assessment can be done by history taking, examinations, and conducting laboratory tests. Common risk factors for poor wound healing include alcohol, smoking, and medical comorbidities (e.g., diabetes and hypertension). Modifying these risks by encouraging lifestyle changes, such as quitting smoking, alcohol moderation etc. or medical interventions are a crucial step in wound management.
Infection Prevention and Control
The rational and appropriate use of antibiotics is the main component controlling infection at a wound site. Prophylactic and therapeutic antibiotics are indicated in the preventive and control stages of wound infection respectively. Satisfactory control of pathogenic microorganisms within the wound area will boost rates of healing with a quicker return of full function.
Wound Cleansing, Debridement, and Dressing
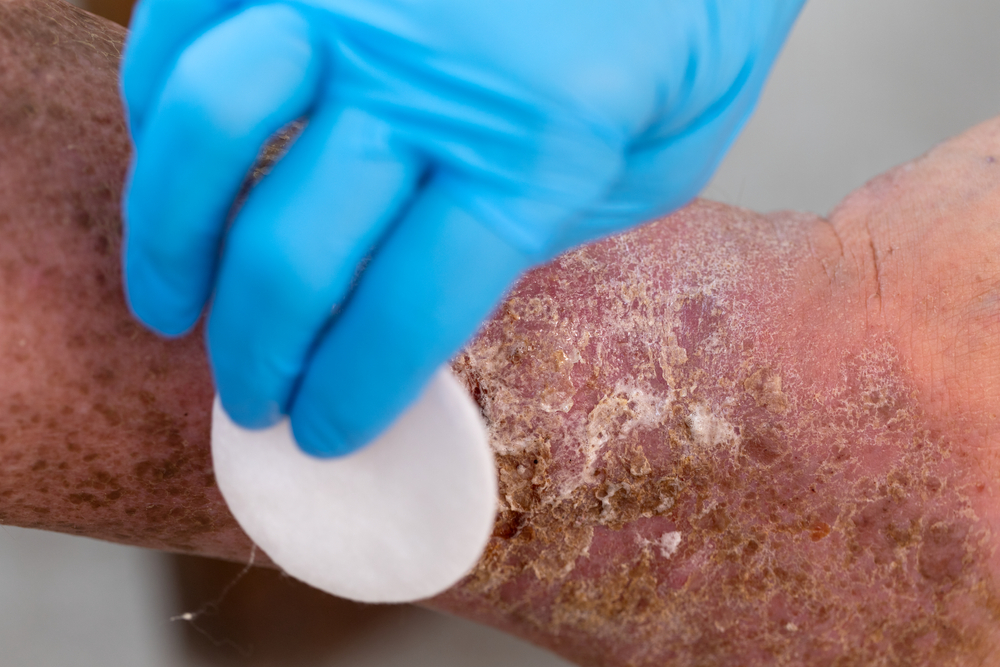
Regularly scheduled local wound care techniques are crucial to achieving satisfactory wound healing outcomes. Timely and consistent wound cleaning with removal of foreign bodies and debridement will ensure the wound site is kept clear of de-vascularized or necrotic tissue which may serve as sources of infectious pathogens. Appropriate wound dressings, such as saline wraps are beneficial in preventing wound infection and stimulating tissue re-epithelialization.
Tissue Perfusion and Moisture Control in Wound Environment
Uninterrupted blood flow to the wound site is a key determinant of successful wound healing as blood conducts oxygen and vital nutrients involved in wound repair to the injury site. Common strategies for improving wound perfusion include moderate exercises and avoidance of occlusive dressings and bandages near the wound site. Further, maintaining a moist wound environment has been shown to contribute to speedy tissue recovery.
Appropriate and Adequate Analgesia
Wound healing can be associated with significant amounts of pain both in acute and chronic wounds.The use of appropriate and adequate amounts of analgesia is a core principle of proper wound care all health professionals must adhere to.
Pain medications should be prescribed using the World Health Organization’s (WHO) pain ladder which advocates a stepwise approach to handling pain. At each rung is the ladder are increasingly potent analgesics corresponding to increasingly severe levels of pain. Pain medications commonly used in managing wounds include non-steroidal anti-inflammatory drugs (NSAIDs), anti-convulsants, and opiates.
Skin Closure
It is often necessary to close gaping skin wounds to hasten wound healing and prevent the formation of unsightly scars. Common methods of skin closure include the use of staples, sutures, and skin and tissue adhesives. Suture placement is the ideal skin closure technique for wounds measuring above 5cm in length while the use of the other methods is limited to smaller wound types.
Nutritional Support
Proper dietary advice should be provided to patients with both acute and chronic wounds as their food choices can determine wound outcomes. Foods rich in antioxidants, vitamins, and bio-flavonoids should form a major portion of the daily intake by patients with healing wounds.
Adjunct Therapy
Other adjunct treatment strategies with limited use by professional healthcare providers include hyperbaric oxygen therapy, electrotherapy, negative pressure wound therapy, and topical re-combinant growth factors.


.webp)

.avif)