80% of all lower limb ulcerations in the United States can be attributed to chronic venous insufficiency. Venous ulcers represent a significant burden to the health care system amounting to annual costs of over $2 billion. Compression therapy is an integral part of wound care and is used in the treatment of chronic venous ulcers. An understanding of the basic principles of compression therapy is essential for wound care specialists and podiatrists.
What Is Compression Therapy?
Compression therapy involves the application of sustained or dynamic pressure to the lower limbs. The pressure is applied using elastic bandages, stockings, or intermittent pneumatic compression pumps and is measured in millimeters of mercury (mm Hg). Even though the degree of pressure applied depends on the diagnosis and presence of comorbidities, an average pressure of 30 to 40 mm Hg is generally recommended. However, for elderly individuals, a pressure of 20 to 30 mm Hg might be sufficient to improve venous return and reduce lower limb edema. The external pressure aids in wound healing by improving venous return, decreasing venous pooling, improving oxygenation and blood flow to the wound site, and reducing edema.
The pressure should be applied in a graded manner, with the highest pressure being exerted at the ankle. Compression therapy requires experience and training, and therefore use of self-bandaging should not be undertaken by the patients. Podiatrists and wound care specialists should ensure that proper technique is employed in compression bandaging as a loose fit can compromise healing.
How Compression Therapy Improves Wound Healing?
As previously discussed, compression therapy is a vital part of wound care for chronic venous ulcers. Patients with chronic venous insufficiency have venous hypertension and lymphedema which delays wound healing. Compression therapy helps to improve wound healing through the following mechanism:
- Improved Venous Return: Compression therapy provides sustained pressure to the lower limb which helps the calf muscles to function effectively as a "muscle pump". This allows for increased venous return to the heart which helps to reduce edema and minimizes pain.
- Improved Microcirculation: Chronic venous insufficiency is characterized by "venous hypertension" which leads to increased ultrafiltration of capillary fluid into the interstitium. Compression therapy helps to counteract this leakage of fluid and improves lymphatic drainage. This improves local blood flow and oxygenation at the wound site which aids healing.
- Release of Vasoactive Mediators: Another important mechanism through which compression therapy aids healing is through the release of vasoactive anti-inflammatory mediators from endothelial cells. This effect has been linked with improved wound healing. In addition, compression therapy is associated with decreased peripheral congestion and tissue remodeling which is important in preventing ulcer recurrence.
Types of Compression Materials
A variety of compression materials and bandages are available that provide a varying degree of compression and pressure to the lower extremities. The initial choice depends on factors like the degree of pain, condition and size of the venous ulcer, and availability. For the majority of patients, elastic, multilayered compression is recommended. Following are the main types of compression bandages and materials available in the market:
- Compression Hosiery: Compression hosiery provides a graded pressure with the highest pressure exerted at the ankle and lowest at the proximal end of the lower limb. It is available in five pressure gradients but the optimal pressure for the treatment of chronic venous insufficiency needs to be at least 20 to 30 mm Hg at the ankle. Compression hosiery is available in various sizes and lengths, but the knee-high compression hosiery is sufficient for most patients. These should be worn with a wound dressing over the ulcer as otherwise, they can be painful.
As the elasticity of compression hosiery decreases with washing and extensive use, they should be replaced after every six months. As leg edema should be minimal when putting on stockings, they should ideally be worn in the morning.
- Compression Bandages: These include elastic and inelastic compression bandages. Inelastic compression bandages are stiff and provide a high working pressure. However, the resting pressure is none. An example of inelastic compression bandaging is the Unna boot which consists of a single bandage that is impregnated with zinc oxide or calamine lotion. It stiffens after application and significantly improves healing rates compared to the placebo. Elastic compression bandages can provide sustained pressure to the lower limbs during ambulation and rest. However, due to the insufficient pressure provided by these bandages, they are not routinely used.
- Multi-Layered Compression Bandage: These consist of 4 layers of bandaging that include padding, crepe bandage, elastic bandage, and a cohesive elastic bandage. Compared to other bandages, they are reasonably well-tolerated by patients and provide pressures within the desired range. Another advantage of multilayered compression bandages is that their application does not require prior extensive training.
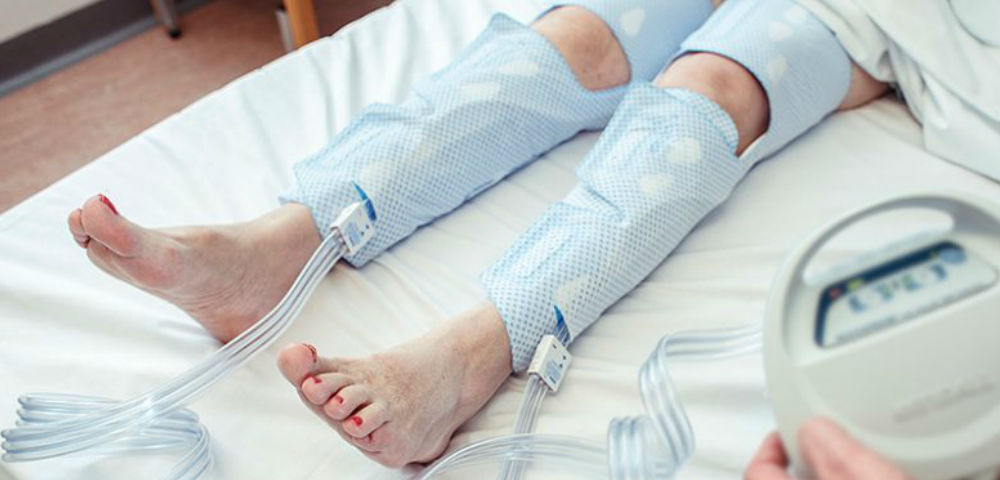
- Intermittent Compression Therapy: Intermittent compression therapy involves the application of external pressure using a cylinder pump that encircles the leg. It periodically inflates and deflates, mimicking the effects of repeated application of compression bandages. Intermittent compression therapy is suitable for patients who cannot tolerate sustained pressure. However, it should be avoided in patients with heart failure and peripheral arterial disease. It enhances wound healing through improved fibrinolysis.
Contraindications To Compression Therapy
Compression therapy is an excellent treatment choice for patients with chronic venous ulcers. However, it is essential to rule out the presence of other conditions that make use of compression therapy unsuitable. Compression therapy is contraindicated in the presence of the following conditions:
- Peripheral Arterial Disease: Compression therapy can compromise the blood supply to the ischemic leg, and therefore should be avoided in patients with the peripheral arterial disease (PAD).
- Heart Failure: Fluid volume shifts can affect the proper functioning of the heart. Therefore, compression therapy should be avoided in these patients.
- Deep Venous Thrombosis: Compression therapy is not recommended in presence of superficial or deep venous thrombosis.
- Cellulitis: Acute skin infections and cellulitis are a contraindication to compression therapy.


.webp)

.avif)