There are several causes of lower extremity ulceration. Venous-stasis wounds, also known as venous ulcer, is a common cause of this ulceration, especially in the United States, where an estimated 500,000 people suffer from the condition. Lack of proper care may lead to higher wound infection chances and other related issues, such as excessive drainage, odor, bleeding, fever, and pains. Patients require adequate care from certified professionals to minimize their chances of infections and health complications.
What Causes Venous-Stasis Wounds?
The primary cause of venous-stasis wounds includes excessive blood pooling in the veins, particularly in the lower extremities. Leaving this health issue untreated for an extended period can lead to infections and severe health complications.
Dysfunctional valves in the vein significantly contribute to venous-stasis wounds. These valves cause blood to flow backward and to pool in the veins, pushing blood cells and other fluids into surrounding tissues. These blood and fluid leakages irritate the tissues, which ultimately cause ulcers or wounds.
Symptoms of Venous-Stasis Wounds
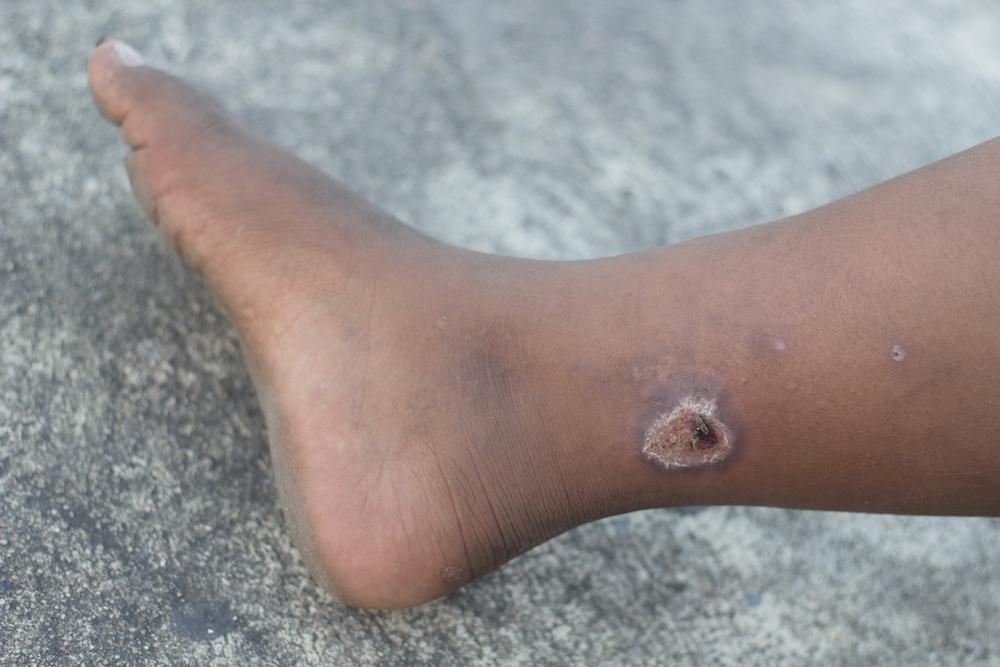
While venous-stasis wounds generally occur on legs and ankles, there are some specific signs and symptoms of this wound type, including:
- Lasting for an extended period of over four (4) weeks
- Discolorations, darkening, and scaly wound edges
- Mild to severe pains in the leg
- Releasing smelling discharges, especially when infected
- Shallow sore sometimes with yellow tissue covering
- Unevenly shaped edges
- Itching and tingling
- Shiny, tight, warm, and discolored periwound skin
Risk Factors for Venous-Stasis Wounds
Although venous-stasis wounds commonly occur in women and older people (i.e., 65 years and above), other factors that can increase the occurrence of this disease include:
- Underlying vein issues, such as varicose veins, deep vein thrombosis, and phlebitis
- Family history of long-term vein disease, e.g., venous insufficiency
- Injury to the leg or veins
- Obesity
- Heart failure
- Pregnancy
- An extended period of inactivity
- Smoking and drug usage
Diagnosis of Venous-Stasis Wounds
Professionals can diagnose venous-stasis wounds by asking about relevant symptoms and patient health history. Moreover, professionals can also perform physical examinations, which often include checking blood flow around the ankle using a blood pressure cuff.
It is noteworthy that identifying the etiology of a wound is critical for venous-stasis wound diagnosis: findings from physical examinations can aid its differentiation from other lower extremity ulcers.
Wound care professionals can also opt for other tests, e.g., plethysmography, ankle-brachial index (ABI) measurement, color duplex ultrasound, etc., for venous-stasis wound diagnosis. These tests are necessary to confirm an unclear preliminary venous-stasis wound diagnosis.
Finally, professionals can leverage the CEAP (i.e., clinical, etiology, anatomy, and pathophysiology) classification system to assess chronic venous disorders. The professionals allocate high CEAP severity scores to patients with chronic, active, and large wounds. Patients with poor prognosis exhibit large-sized venous ulcers over a prolonged duration.
Venous-Stasis Wound Treatment
Conservative management, mechanical treatment, medications, and surgical management are some treatment options for venous-stasis wounds. Although each treatment option aims to reduce edema, improve wound healing, and prevent a recurrence, they exhibit variable effectiveness.
Conservative Management
Conservative management techniques, such as compression therapy, leg elevation, and dressings, can significantly improve patients with venous-stasis wounds.
Compression therapy methods, including inelastic, elastic, and intermittent pneumatic compression, improve venous reflux, reduce pains and edema, and enhance wound healing with success rates ranging from 30% to 60% at 24 weeks and 70% - 85% at 12 months. Consistent adherence to the therapy also minimizes the recurrence chances after wound healing.
While inelastic compression therapy offers high working pressure during muscle contraction and ambulation without resting pressure, elastic compression therapy conforms to leg size changes and sustains compression during rest and activities.
Conversely, intermittent pneumatic compression leverages a pump for air delivery into inflatable and deflatable sleeves that provide compression to the extremities at intervals.
An integration of compression therapy with leg elevation includes a standard method of care professionals leverage for the treatment of venous-stasis wounds. This method reduces edema, improves microcirculation and oxygen delivery, and expedites wound healing by raising the lower extremities above the heart level.
Patients experience significant improvements with 30 minutes of leg elevation four times daily. The method increases blood flow within the veins by up to 45%, making it an essential treatment option for the disease.
Moreover, applying dressings under compression bandages promotes faster healing and minimizes bandage adherence to the wound. Factors such as cost, ease of application, and preference of the patient and wound care professional affect the choice of dressings for venous-stasis wounds.
Medications
Health professionals can opt for medications that offer several improvements for the overall venous-stasis wound healing process, such as improving blood flow, reducing pains, preventing pains, etc. Some options include:
- Pentoxifylline for lowering blood viscosity and improving microcirculation
- Aspirin for minimizing healing time and wound size
- Iloprost for inhibiting platelet aggregation and reduced healing time
- Antibiotics/antiseptics
- Hyperbaric oxygen therapy
Surgical Management
Since chronic venous-stasis wounds have a poor healing rate of about 22%, professionals may consider surgical treatment options, such as debridement, skin grafting, etc.
Preventing Venous-Stasis Wounds
A proactive approach can significantly prevent the recurrence of venous-stasis wounds. Patients must take measures to improve blood flow and minimize the occurrence of dysfunctional valves. Patients must consider some lifestyle changes, including:
- Consistent use of compression stockings
- Staying physically active to improve blood flow
- Minimizing or quitting smoking
- Weight control to avoid obesity
- Reducing sugar levels, especially in diabetic patients
- Eating healthy and getting sufficient rest
- Managing blood pressure and cholesterol levels
Bottom Line
Venous-stasis wounds can lead to severe health complications if left untreated over a prolonged duration. Identifying its causes and symptoms includes the first steps to effectively managing and treating the disease. Wound care professionals can opt for conservative, medication, or surgical treatment options depending on the nature of the wound. Moreover, studies have shown that integrating several options can significantly expedite wound healing and maximize patient comfort.


.webp)

.avif)