Edema results from the inability of the body's drainage mechanism to eliminate excess fluid within skin cells and tissues, leading to the swelling and enlargement of the affected body part. This condition is prevalent in patients with chronic wounds. While an estimated 2% of the US population suffers from chronic wounds, there is a strong relationship between edema and chronic wounds. Consequently, wound care professionals must understand the symptoms, causes, and treatment options of edema to provide adequate care to chronic wound patients.
What is Edema?
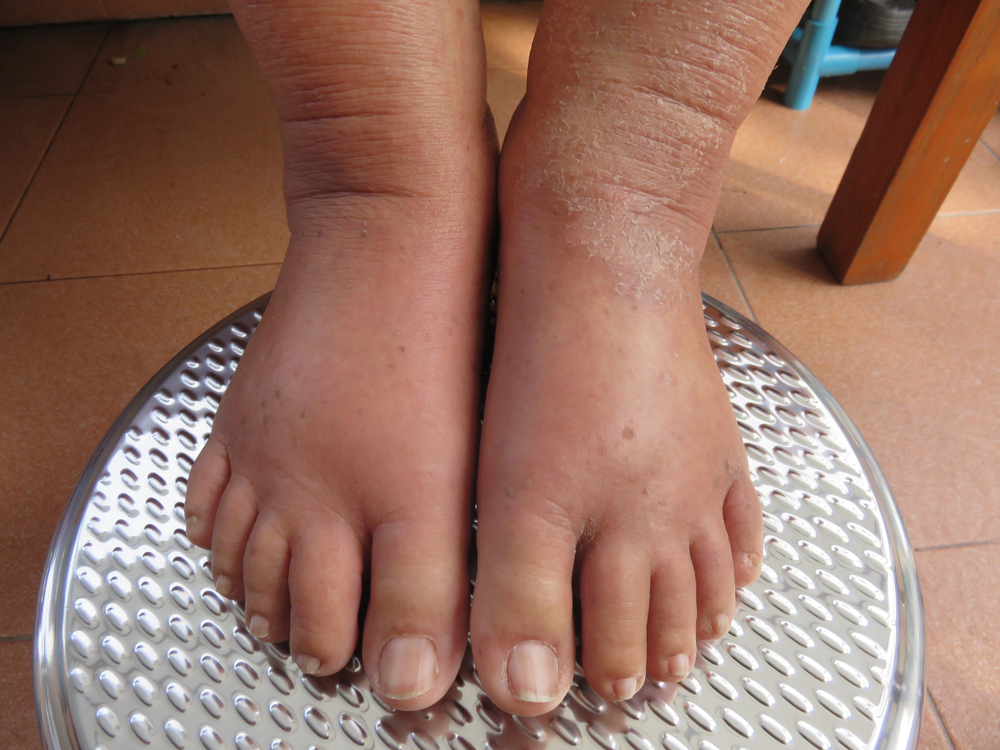
Edema includes a medical condition involving swelling from trapped fluid in body tissues. This condition regularly occurs around the ankles, feet, and legs, affecting several other body parts, including the hands, face, and abdomen.
Edema prevalence is high due to its association with several underlying health conditions. Since mild cases of edema disappear without medication, it is relatively difficult to project its occurrence rate.
Five types of edema, categorized according to the body part it affects, include peripheral, pleural, pulmonary, cerebral, and anasarca edema. Patients with chronic wounds develop edema around the wound site depending on the presence or absence of underlying health conditions. Thus, chronic wound patients are most susceptible to peripheral edema.
Edema occurs through excess interstitial fluid movement to spaces between body cells and tissues. The inability of the natural drainage mechanism in the body to eliminate this excess fluid leads to body swellings in affected areas, such as chronic wound sites.
Symptoms of Edema in Chronic Wounds
Significant swelling or enlargement of the affected body part is the primary symptom of edema in chronic wounds. Other symptoms of the condition include:
- Skin with a shiny appearance
- Skin tissue puffiness or swelling, especially in the legs and arms
- Walking difficulties due to swelling
- Mild pain or sore feeling around the wound site
- Significant weight gain
- Breathing difficulty in extreme cases
- Tightness around the wound site
- Skin with dimples or pits, especially after pressing for several seconds
Risk Factors of Edema
Some risk factors that alter interstitial fluid dynamics and result in edema in chronic wounds include:
- Surgery
- Burns and other tissue traumas
- Kidney disease
- Severe protein deficiency
- Several types of medications, including steroids, high blood pressure, estrogen, anti-inflammatory, and diabetic medications
- Lymphatic system defects
- Chronic wounds
- Insect bites and stings
- Heart failure
Causes of Edema
The primary causes of edema include fluid leakage from tiny blood vessels (or capillaries) in the human body and the inability of the body's drainage mechanism to eliminate such fluids. Some other causes of this condition include:
- Physical immobility for an extended period
- Side effects from certain medications
- Excess intake of salt and salty foods
- Underlying health issues, e.g., kidney disease
- Poor nutrition
- Weakened veins and other body vessels
- Pregnancy
- Compromised immune system
Treatment Options for Edema
Several treatment options for edema include medication, affected body part elevation, underlying medical condition control, compression wears, and exercise and ambulation. These options are among the most effective for edema management.
Medication
Analstegia, antihistamines, and diuretics are some of the most effective medications for edema management. Chronic wound patients with edema are susceptible to mild to extreme pains. The use of Non-steroidal anti-inflammatory drugs (NSAIDs) or mild opioid analgesia can efficiently address this issue.
Moreover, while antihistamines can adequately treat allergy-related edema, diuretics can reduce edema through urine excretion. It is noteworthy that antihistamines stabilize affected cells, eliminating pro-inflammatory chemical mediator release.
Elevation of Affected Body Part
Elevating the edematous area can efficiently relieve pressure in that area, consequently leading to reduced fluid pooling. Wound care professionals can incorporate this option into the patient treatment and emphasize the need for body part elevation.
Control of Underlying Medical Condition
Professionals must also account for the effects of underlying medical conditions in wound patients with edema. Patients can experience better outcomes with adequate management of these underlying issues and achieve significant edema reduction.
Use of Compression Wears
Compression wear, such as socks, sleeves, or gloves, can efficiently minimize the further development of edema. Professionals typically consider this option in the advanced stage of edema treatment to minimize fluid re-accumulation around the affected wound site.
Exercise and Ambulation
Mild to moderate workouts and regular ambulation can improve venous circulation in the affected areas and improve lymphatic training of fluids, significantly reducing swellings or enlargements.
Preventing Edema
While underlying health issues and chronic wound conditions significantly contribute to edema development, patients can meet wound care professionals to identify the most appropriate option for managing the symptoms. Patients must consider altering their nutrition to minimize excess salt intake.
Moreover, exercise and regular physical activities are essential for preventing edema, as prolonged immobility significantly contributes to its development.
Bottom Line
Chronic wound patients are susceptible to edema. Some key symptoms of the condition include swelling, mild pain, skin shininess, tightness around the wound site, and significant weight gain. In addition to the damage to body drainage mechanism, nutrition, underlying health conditions, prolonged immobility, and side effects from medications are some causes of edema. Finally, the top treatment options for edema include medications, body part elevation, control of the underlying medical condition, compression wears, and exercise and ambulation.


.webp)

.avif)