Patients with severe burns or wounds due to trauma, typically require skin grafts to facilitate faster tissue recovery. A lot of the donor skin tissue used in wound grafting procedures are allografts sourced from unaffected body sites. The wounds resulting from tissue harvest at these donor sites also require wound care as they are prone to various healing complications.
Skin Grafting Basics
Skin grafting involves the transfer of healthy vitalized skin tissue from a suitable donor site to another body location that has been damaged by burns or other forms of physical trauma. A skin graft is a section of the epidermis, and dermis that is used to correct a defect in a recipient skin site. Depending on the depth of skin tissue harvested from the donor sites, skin grafts can be considered as partial thickness or full thickness. In keeping with best practices governing wound healing regardless of etiology, the more extensive the tissue harvest is, the more post-transplant wound care the donor site will require.
Categorizing Skin Grafts
Skin grafts generally fall into split thickness or full-thickness types. Below is a closer look at the two categories:
Split Thickness Skin Grafts
A split-thickness skin graft is one where the entire epidermis and the upper part of the dermis are removed from the donor site for transplantation. In this type of graft, the procedure leaves just enough dermis to sustain reepithelialization. While these grafts can be used on recipient graft beds with poor vascularity, they provide poor cosmesis after the wound resolution.
Full-Thickness Skin Grafts
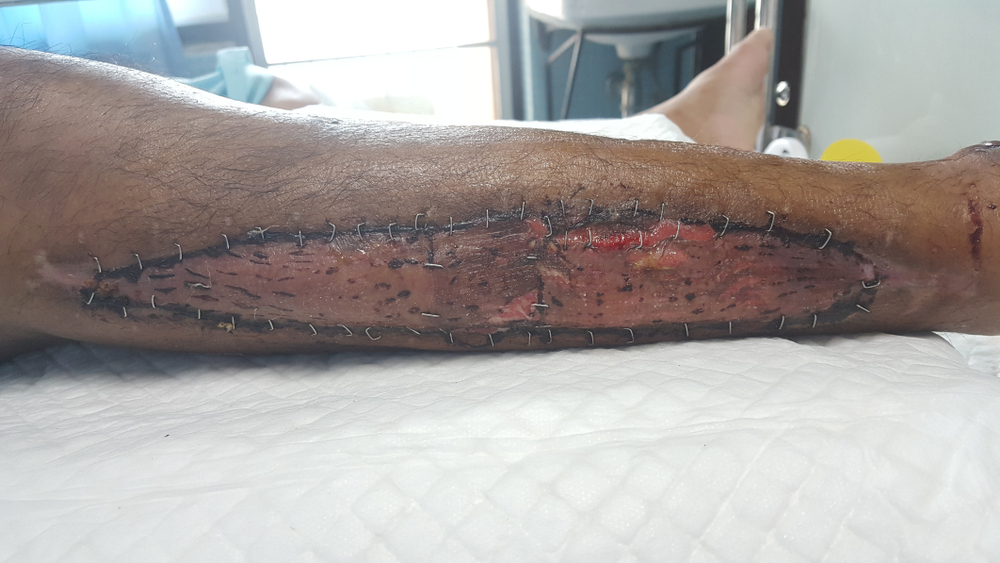
Full-thickness tissue grafts transplant the entire epidermis, and dermis from a donor site to a recipient wound bed. Closing a defect with a full-thickness graft provides a better cosmetic look after grafting is completed. This is because full-thickness grafts retain as much of the original skin make-up as possible. Although they are highly aesthetical, full-thickness grafts are limited to the correction of small wound defects due to the disruption they cause at the donor sites.
Why Is Donor Site Wound Care Crucial?
Despite its obvious benefits, the removal of skin tissue from a donor site is a traumatic event that has negative effects if proper care is neglected. A donor wound site will undergo all the stages of wound healing expected in any wound type regardless of its etiology. Donor wounds are prone to microbial colonization with infection and cause transplant patients significant tissue swelling, pain, and deformity. Thus, wound care experts offering their patients tissue grafting options must provide an optimal healing environment for both the recipient beds, as well as the donor sites.
Complications Affecting Skin Graft Donor Sites
The complications affecting skin graft donor sites are similar to that of the recipient sites.
- Bleeding with the formation of blood collections (hematomas) within the wound site
- Colonization by microorganisms with the onset of infection
- Undesirable healing outcomes (scarring with poor scar cosmesis)
- Persistent pain even after wound resolution
Wound Care Techniques in Skin Grafting
Good wound healing practice, mandates wound care professionals to provide appropriate care for both the recipient and donor sites. Depending on the type of graft harvested, the components of managing wound healing at the donor site will vary. While split-thickness skin grafts heal by reepithelialization, defects left behind after removing full-thickness grafts must be sutured together and allowed to heal by primary intention. Effective wound care techniques for skin graft donor sites regardless of the nature of tissue harvested include the following:
- Analgesia
- Antibiotics
- Wound dressing
- Emollients
Analgesia
The pain experienced by patients undergoing skin grafting is considerably worse at the donor sites due to the exposure of nerve endings following tissue harvest. Wound care must include the use of sufficient amounts of pain medications to make the post-graft period as comfortable as possible for the patient.
Antibiotics
Due to an increased risk of infection following skin harvest, infection control can be achieved by the use of prophylactic antibiotics. This will inhibit microbial proliferation at the wound site and aid optimal tissue healing.
Wound Dressing
Proper local wound care is key to preventing complications at the donor site. Moist wound dressings are particularly effective in the treatment of split-thickness graft donor sites. Moist dressings will prevent drying at the donor site and therefore prevent further mechanical damage and tissue loss.
Emollients
Newly healed donor sites tend to be quite dry and itchy. This makes them prone to repeated scratching by graft patients leading to repeat trauma, and possible infection. Consequently, skin graft patients should be strongly counseled not to scratch healed donor sites to avoid further trauma to the healed site. Wound care experts can circumvent this challenge by prescribing skin emollients that moisten dry skin and ease itchiness. Further, oral antihistamines can be prescribed to limit itching at donor sites however, patients must be counseled on possible side effects such as drowsiness.


.webp)

.avif)