Wound debridement is a critical component of the wound healing process that sets the stage for re-epithelialization. In chronic wounds, such as pressure ulcers, venous ulcers, and diabetic foot ulcers, proper and timely debridement can significantly improve the rate of healing. This article discusses what wound debridement is, how it works, and the various methods applied in today's clinical practice.
What is Debridement in Wound Management?
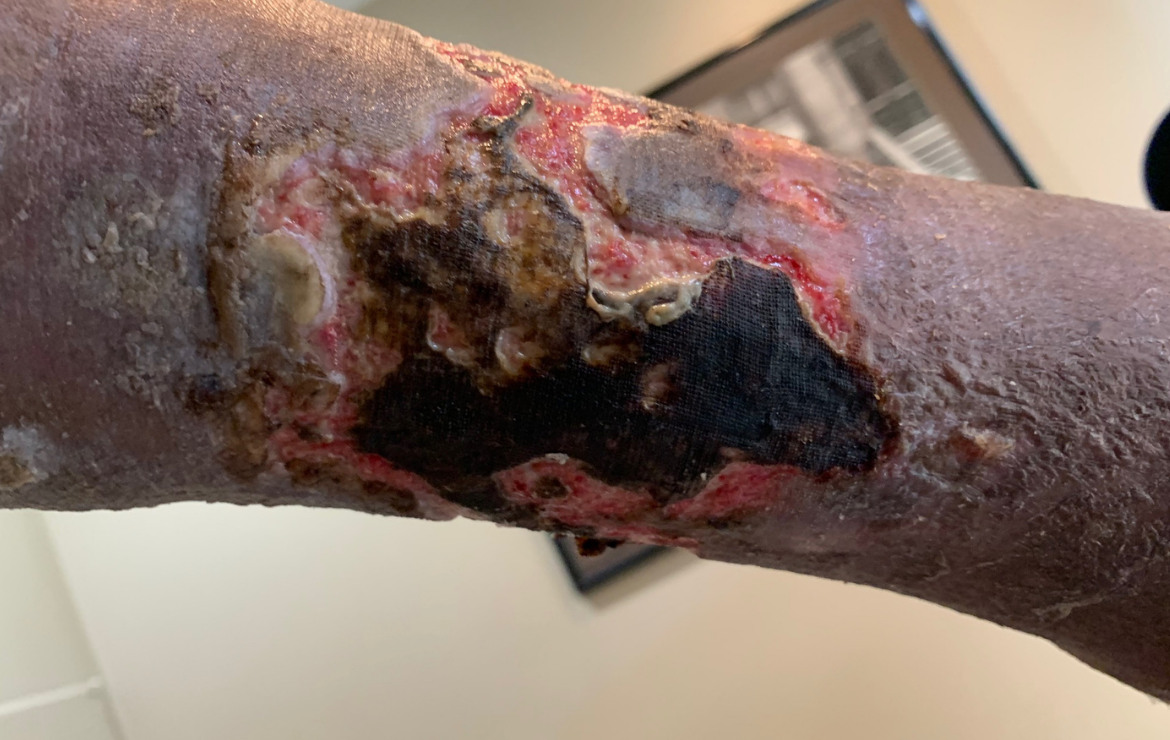
Wound debridement is the removal of devitalized or dead (necrotic) tissue and foreign materials from the wound bed to aid healing. Necrotic tissue forms as slough or eschar on the surface of the wound. Slough appears as a yellowish, soft tissue made up of liquefied dead tissue, debris, dead white blood cells, and fibrin, which develops during the inflammatory phase. Eschar appears as dry, black scabs that form when dead skin cells agglomerate. Debridement is a part of the standard DIME technique for wound bed preparation in chronic wounds, which includes:
- D: Debridement of necrotic tissue.
- I: Infection and inflammation management
- M: Moisture control
- E: Epithelial assessment
Why is Debridement Necessary?
The presence of necrotic tissue in wounds can prevent or slow the rate of healing. The following are some justifications for debridement:
- Necrotic tissue can serve as viable cultures for bacteria, which can result in infection and odor.
- Dead tissue acts as a barrier to angiogenesis (formation of new blood vessels) as well as the development of granular tissue and new extracellular matrix (ECM).
- Removing necrotic tissue from a wound can reveal underlying infection not immediately apparent during wound assessment.
- Removing slough and eschar allows applied topical agents to reach the wound bed
- Removing devitalized tissue helps to keep wounds clean and free of debris.
Debridement Methods for Wound Management
Current debridement methods for wound care include autolytic, biological, enzymatic, mechanical, and surgical (sharp) debridement. In this section, we examine each of these methods in closer detail:
Autolytic Debridement
Autolytic debridement uses the body's natural moisture and enzymes to break down slough and eschar. This technique uses moisture-donating or retentive dressings to soften and eventually aid the separation of necrotic tissue from the wound bed. Suitable dressings include films (semi-occlusive or occlusive), hydrogels, and hydrocolloids. Wound dressings help maintain a moist environment to facilitate debridement. A key benefit is that it is highly selective, only affecting devitalized tissue. Autolytic debridement is ideal for non-infected injuries, especially in patients with healthy immune systems. However, it can serve as adjunctive therapy for managing infected wounds.
Biological Debridement
Also known as larval therapy, biological debridement involves the use of maggots cultured in a sterile environment to break down necrotic tissue. The sterile larvae are applied to the wound bed using dressings. The organisms secrete enzymes that dissolve dead tissue in the wound matrix to prepare them for ingestion. Biological debridement is especially beneficial in wounds with large surface areas and is relatively painless compared to other methods. However, it is not suitable for use in patients under immunosuppression therapy and close to septic areas.
Enzymatic Debridement
Enzymatic debridement involves using topical agents containing natural proteolytic enzymes such as collagenase, to break down slough and eschar. It can be performed in conjunction with surgical (sharp) debridement with topical agents widely available in the pharmaceutical industry. Enzymatic debridement is a selective technique that targets only necrotic tissue. It is suitable for managing chronic wounds, such as diabetic ulcers, venous ulcers, pressure ulcers, and infected wounds. However, enzymatic debridement products may be contraindicated for use in patients that exhibit sensitivities to any of the ingredients.
Mechanical Debridement
This technique is a cost-effective method of debridement suitable for acute and chronic wounds. It involves the use of hydrotherapy, wet-to-dry dressings, or negative-pressure wound therapy (NPWT) to separate slough and eschar from the wound bed. However, unlike other techniques, mechanical debridement is non-selective, removing both necrotic and viable tissues.
Surgical (sharp) debridement
Surgical debridement involves the use of sharp instruments, including scalpels, curettes, scissors, and Metzenbaums, to remove necrotic and dry tissues from wounds. Wound care clinicians can perform surgical debridement in operating theaters or at the bedside. It usually requires local anesthesia and specialized techniques to control bleeding.
Surgical debridement is a favored method for wound bed preparation for the following reasons:
- It creates the initial trauma necessary to "reset" the wound healing process into the inflammatory phase
- Facilitates wound healing by removing both biofilm and dead tissue
- Allows clinicians to ascertain the depth and severity of wounds as well as identifying underlying infection
- Suitable for removing large areas of dead tissue from wounds


.webp)

.avif)