One of the most serious complications patients with prolonged wounds develop is tunneling or sinus tracts. These injuries pose a serious threat to early tissue recovery as they comprise body tissues that result in impaired wound closure. Due to the seriousness of this condition, wound care professionals must be able to recognize and treat tunneling wounds promptly.
What are Tunneling Wounds?
Tunneling wounds or sinus tracts are a category of complex wounds that extend from the skin surface to various underlying tissues. Tunneling wounds are also known as tracking wounds because they form “passageways” between the skin and various subcutaneous structures in an irregular manner. Due to the random manner in which they form subdermal defects, tunneling wounds can create dead spaces that have the potential to become abscess cavities when an infection occurs. Further, tunneling wounds may cause poor wound resolution due to damage to multiple tissues associated with the initial injury. The result is a significantly higher likelihood of infection, edema, and wound breakdown.
Etiology and Risk Factors
There are a host of intrinsic and extrinsic wound aetiologies and risk factors that can contribute to the development of tunneling wounds in susceptible patients which include:
- Infection at the acute or chronic wound site
- Delayed wound healing from protracted tissue inflammation
- Tissue trauma resulting in shear or pressure injuries
- Poorly controlled wound moisture
- Irrational use of antibiotics with development of resistant strains of bacteria
- Corticosteroid use inhibiting the formation of collagen critical to wound repair processes
- Patients with chronic medical conditions, such as diabetes that slow healing and increase risk of wound infection
- Obesity
- Malnutrition
- Cancer chemotherapy and use of immunosuppressant medications
- Previous surgery around the wound site
- Obesity
- Malnutrition
- Cancer chemotherapy and use of immunosuppressant medications
- Previous surgery around the wound site
Clinical Features
The clinical features seen in patients with tracking wounds are:
- Fever
- Pain around the wound site
- Soft tissue swelling within and around the injury site
- Purulent, foul-smelling discharge from the wound site
- Redness of affected skin area
- Signs of maceration with whitish, friable skin
The typical presentation of a tunneling wound is on with an externally visible lesion that may communicate with one wound site or track beneath the skin surface to end blindly within subcutaneous fat, muscles, or connective tissues.
Diagnosing Tunneling Wounds
The diagnosis of tunneling wounds clinically requires a close physical examination of the wound site followed by laboratory and radiological investigations. While some patients will present with wounds that have easily recognizable tracts and communications, others may have wounds with obscure passageways. In the latter scenario, wound care physicians will have to probe the wound to determine the extent of the sinus.
Useful Imaging Modalities
To aid an accurate diagnosis of a tunneling wound, wound care experts can employ different diagnostic imaging techniques. Manual probing can be done after giving the patient adequate analgesia. Flexible polythene catheters are ideal for assessing wound direction and determining depth. Also, ultrasonography, magnetic resonance imaging, and computerized tomography scanning can be used to delineate the true extent of tunnel wounds. This will enable wound care providers to plan and implement effective strategies to optimize wound healing.
Wound Management Approaches in Tunneling Wounds
The application of strict wound care techniques is essential to the resolution of all forms of tunneling wounds. Some key approaches to treating tracking wounds are outlined below:
- Removal/Management of identifiable causes
- Symptom control with appropriate medications
- Wound cleansing, drainage, packing, and dressing
- Limb resting, avoidance of pressure at wound sites
- Negative pressure wound therapy
- Surgical intervention
Removal/Management of Identifiable Causes
An important first step in treating tunneling wounds is the elimination of the initial cause. Removal of the patient from traumatic stimuli, management of chronic medical diseases, and adoption of healthier lifestyle choices are ways of mitigating wound causes.
Symptom Control with Appropriate Medications
Wound care providers must provide the appropriate class of drugs for each of the symptoms their patients present with. Commonly employed drug classes include:
- Antibiotics for infection control
- Analgesia for manage pain
- Phenols to treat pilonidal cysts
Wound Cleansing, Drainage, Packing, and Dressing
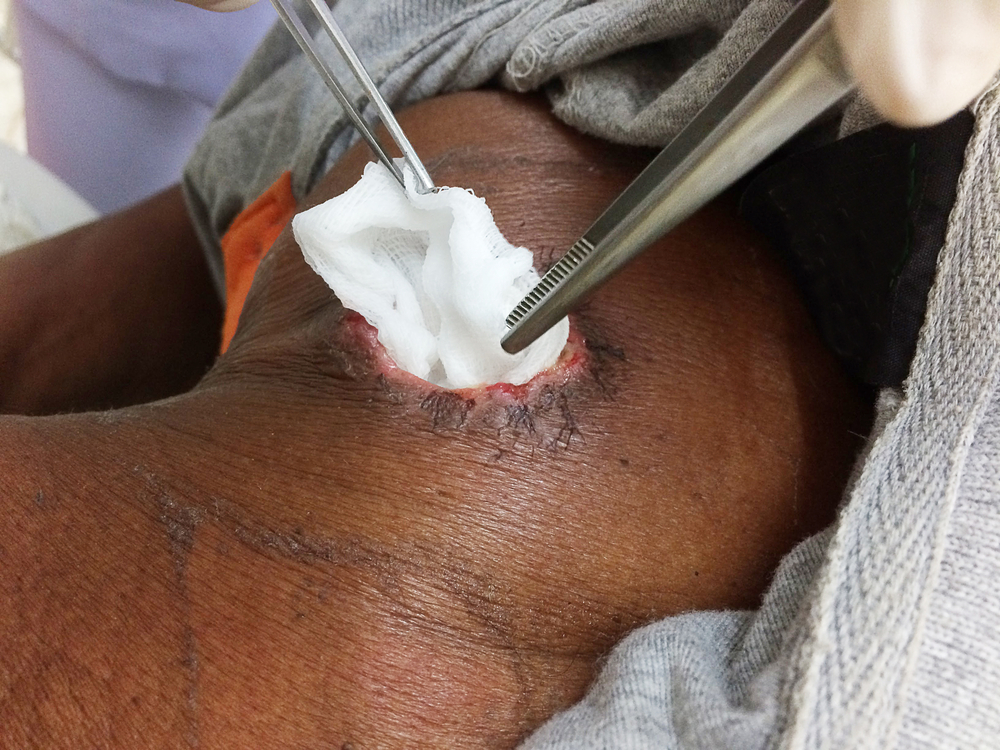
Proper care for wound sites will help optimize the healing process in patients with tunneling wounds. Wound care providers must ensure their patients have their injuries properly cleansed, and drained with tracts firmly packed to reduce the risk of abscess formation. Further, the use of alginates, collagen dressings, and hydrogels are recommended to optimize tissue recovery.
Limb Resting, Avoidance of Pressure at Wound Sites
Patients should be encouraged to rest their limbs as often as possible to reduce the amount of weight reaching the wound sites.
Negative Pressure Wound Therapy
Negative pressure wound therapy or vacuum-assisted wound closure is used to limit the amount of air pressure at the wound surface which creates a hostile environment for disease-causing bacteria while improving the rate of wound recovery.
Surgical Intervention
In some cases, it is necessary to surgically incise the wound tract and leave them open to heal. This technique provides better access to the wound tract and makes wound care easier.


.webp)

.avif)