Chronic wounds, including diabetic ulcers, venous insufficiency ulcers, and arterial leg ulcers, are on the increase due to risk factors, such as aging populations, obesity, and diabetes. Since these wounds do not heal quickly and often recur, they place a significant burden on limited healthcare resources for their adequate management. Timely intervention, regular wound care, and continuous patient education can improve healing outcomes in patients.
What Is An Arterial Leg Ulcer?
Arterial leg ulcers (ALUs) are open wounds on the lower extremities caused by arterial insufficiency; inadequate supply of blood through the coronary arteries. According to research, ALU affects 0.6 to 3% of people over 60 years of age and increases to 5% in people over 80 years old. Nonetheless, ALU is, however, not limited to older populations; risk factors and comorbidities, e.g., peripheral artery disease and diabetes, can affect adults of any age.
Low perfusion to the lower extremities may result from the buildup of fats in or the hardening of the arteries and causes constriction. Tissue neuropathy follows in the affected limb, which forms an open wound. If ALUs are left untreated, they may become infected with widespread tissue necrosis, which can necessitate limb amputation.
Symptoms and Diagnosis
Venous ulcers exhibit many similar symptoms as arterial ulcers, such as inflammation and swelling. Knowing the difference can be critical for preventing a misdiagnosis. The main distinction from an etiological standpoint is that arterial ulcers result from poor blood circulation via the arteries, while venous ulcers are due to restricted supply through the veins.
Symptoms of ALUs include but are not limited to:
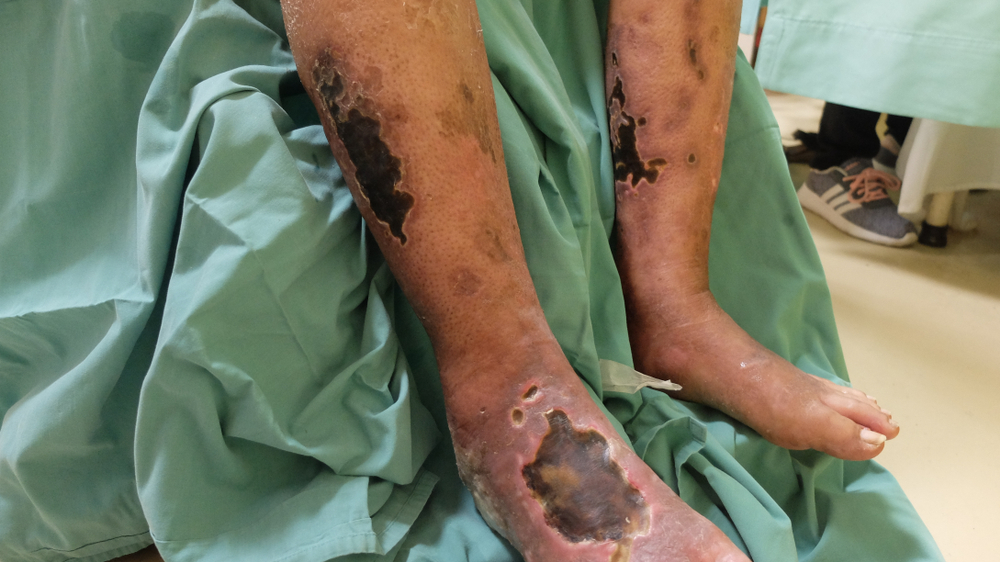
- Open wounds on the heels, ankles, or on the tips of the toes
- Wounds having a "punched-out" look
- Well defined wound margins
- A non-bleeding wound bed with a black, red,
- Pale peri-wound skin that appears glossy
- Hair loss in the affected skin
- Delayed capillary return in the affected limb(s)
- Pain in the affected area that worsens at night or when elevated
- Limbs feel cold to the touch with a weak or absent pulse
- Nails and skin on the affected limbs appear pale or darker than usual
Diagnosing ALUs involves determining the wound etiology and reviewing a patient's medical history to identify risk factors. While the use of antibiotics prevents infection, identifying the underlying causes can improve outcomes and avoid a recurrence. Tests for diagnosing arterial insufficiency in patients include:
- Capillary refill time: Involves applying positive pressure to a part of the affected extremity and noting the time it takes for blood vessels in the skin to refill. A delayed capillary return indicates low perfusion.
- Buerger test: The clinician elevates the patient's feet 45 degrees for 60 seconds with the patient in a prone position. A limb that becomes pale when elevated and turns red when lowered may indicate arterial insufficiency.
- Ankle Brachial Pressure Index (ABPI): The clinician uses a Doppler probe to calculate ABPI. This test measures the ratio of blood pressure in the ankle to that of the brachium. A value than 0.9 indicates low perfusion, likely caused by peripheral artery disease.
- Transcutaneous oximetry: A non-invasive test for measuring the oxygen content of tissues; here, a clinician first removes any wound dressings present, cleans the affected site with alcohol, and applies an electrically-conductive gel to the wound. Then, the clinician uses a special sensory apparatus to calculate the oxygen content of the affected limb. This test is especially helpful for determining the severity of blood flow deprivation due to advanced peripheral arterial disease.
Risk Factors for Arterial Leg Ulcers
Common risk factors for ALUs include, but are not limited to, the following:
- Diabetes Mellitus
- Old age
- Obesity
- Smoking
- High body fat and cholesterol
- Renal failure
- Rheumatoid arthritis
- Hypertension
- Vasculitis
- Heart diseases
- Peripheral vascular disease
Treatment and Wound Care for Arterial Leg Ulcers
The standard clinical treatments for ALUs are angioplasty and stent placement. The primary objective of treatment is to improve blood circulation in the affected extremity by minimizing constriction in affected arteries. The procedure involves the use of tiny medical balloons to open constricted or blocked coronary arteries. Stents are tiny, wire-mesh structures that prevent the vessel from closing again. Lifestyle modifications can also address the underlying factors that contribute to ALU development or recurrence. For example, quitting smoking and switching to a healthier diet with lower unsaturated fats/cholesterol can reduce blood lipid levels that often result in clogged arteries. If infection occurs, antibiotics can help. Wound care professionals should also change dressings frequently and perform debridement as healing progresses.


.webp)

.avif)